Maintaining a comprehensive understanding of the uninsured population is more than a statistical exercise; it is a critical necessity for public health stability. For those of us in the medical community, the gap between needing care and having the means to access it often defines the trajectory of a patient’s health. In the United States, tracking who lacks health insurance and why is a complex operation that relies on rigorous data collection to inform policy and clinical outreach.
To understand the current state of healthcare access, we must look at the mechanisms used to identify the uninsured. The process involves a sophisticated blend of government surveying and independent analysis, ensuring that policymakers have a clear picture of the social and economic barriers preventing millions from receiving essential medical services.
As a physician and journalist, I have seen how data-driven insights can lead to targeted interventions. By identifying specific demographics or geographic regions with high rates of uninsured residents, health systems can better allocate resources, expand community clinics, and advocate for policy shifts that protect the most vulnerable populations.
The American Community Survey: The Gold Standard for Coverage Data
The primary engine for tracking health insurance status in the United States is the American Community Survey (ACS). Conducted by the U.S. Census Bureau since 2005, the ACS serves as the premier source of detailed information regarding the nation’s people and housing. Unlike the decennial census, which provides a broad snapshot every ten years, the ACS is an ongoing survey that provides annual estimates, allowing for a more responsive understanding of how coverage trends shift year over year.

The ACS is designed to capture a holistic view of the resident’s life. It collects detailed social, economic, and demographic information, which is essential because health insurance status does not exist in a vacuum. By gathering data on income, education, and employment alongside health insurance coverage, the survey allows researchers to see the correlation between economic instability and the lack of medical protection.
This data is comprehensive in scope. The ACS covers U.S. Residents across all 3,141 counties in the 50 states, the District of Columbia, and all 78 municipalities in Puerto Rico. Importantly, the survey includes not only those living in residential housing but likewise individuals residing in group quarters facilities, ensuring that marginalized populations are not excluded from the count.
The Mechanics of Data Collection
For data to be authoritative, the methodology must be robust. The U.S. Census Bureau employs a multi-modal approach to ensure a high response rate and accurate representation of the population. The data collection operation utilizes up to four different modes: internet questionnaires, mail-in options, telephone interviews, and personal visit interviews.
The process typically begins with a mailed request for the resident to respond via the internet. If that is unsuccessful, a paper questionnaire is offered. For those who still do not respond, the Bureau attempts follow-up interviews by phone or in person. This layered approach is vital for reaching populations that may lack reliable internet access or stable housing, who are often the same individuals most likely to be part of the uninsured population.
The resulting data provides annual estimates for states and specific geographic areas with populations of 65,000 or more. This granularity allows public health officials to identify “healthcare deserts” or regions where insurance penetration has dropped, enabling a more surgical approach to public health interventions.
Translating Census Data into Public Health Action
While the U.S. Census Bureau collects the raw data, the true utility of the ACS is realized through expert analysis. Organizations such as KFF (Kaiser Family Foundation) play a pivotal role in this ecosystem. By analyzing a 1% sample of the U.S. Population from the ACS, KFF provides detailed analysis on health insurance status and the total population’s coverage levels.
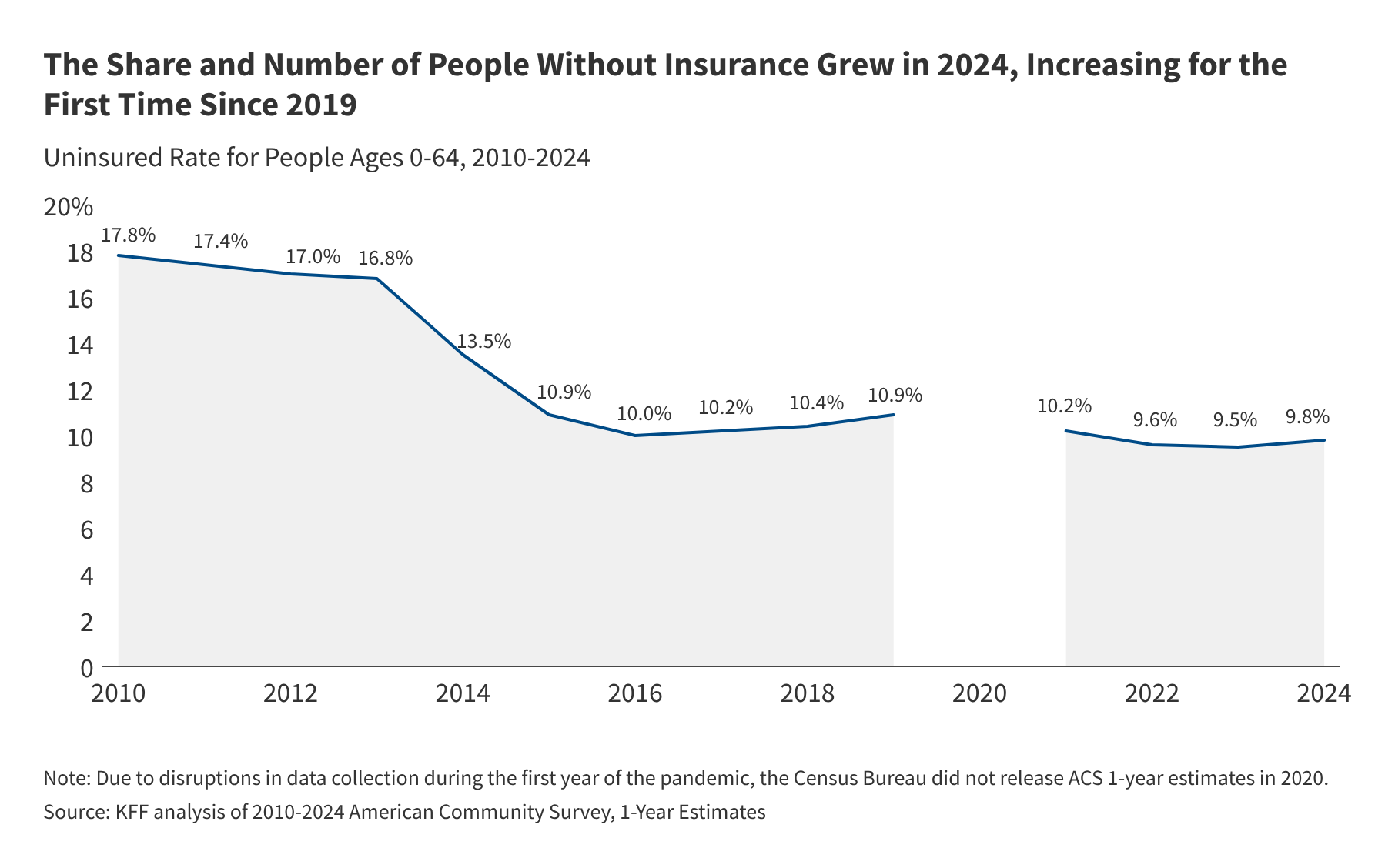
This translation of raw data into “issue briefs” and policy indicators is what allows the medical community and legislators to understand the financial implications of being uninsured. When analysis reveals a growth in the uninsured share of the population, it signals a potential increase in delayed care, higher emergency room utilization, and a rise in untreated chronic conditions.
From a clinical perspective, these statistics are a warning light. An increase in the uninsured population typically correlates with a decline in preventive screenings and early interventions. For a physician, this means seeing patients in more advanced stages of disease, which is both more challenging to treat and more costly for the healthcare system at large.
Key Components of ACS Health Data
To better understand what the ACS tracks regarding the uninsured, it is helpful to look at the specific data points collected annually:
- Demographic Characteristics: Age, race, and ethnicity to identify which groups are most affected by coverage gaps.
- Economic Indicators: Income and occupation levels to determine the affordability of private insurance.
- Housing Characteristics: Type of housing and conditions, which often overlap with social determinants of health.
- Coverage Status: Direct estimates of who possesses health insurance and the type of coverage they hold.
By synthesizing these factors, the ACS provides a map of the systemic failures in the healthcare delivery system, highlighting exactly where the safety net has frayed.
As we look forward, the continued accuracy of these surveys remains paramount. The next official updates to these datasets will continue to guide the evolution of healthcare policy and the expansion of access for those currently left behind. For those seeking the most current data on their specific region, the U.S. Census Bureau’s official portals remain the most reliable point of entry.
Do you believe current data collection methods are sufficient to capture the needs of the most marginalized populations? Share your thoughts in the comments below or share this article to join the conversation on healthcare access.