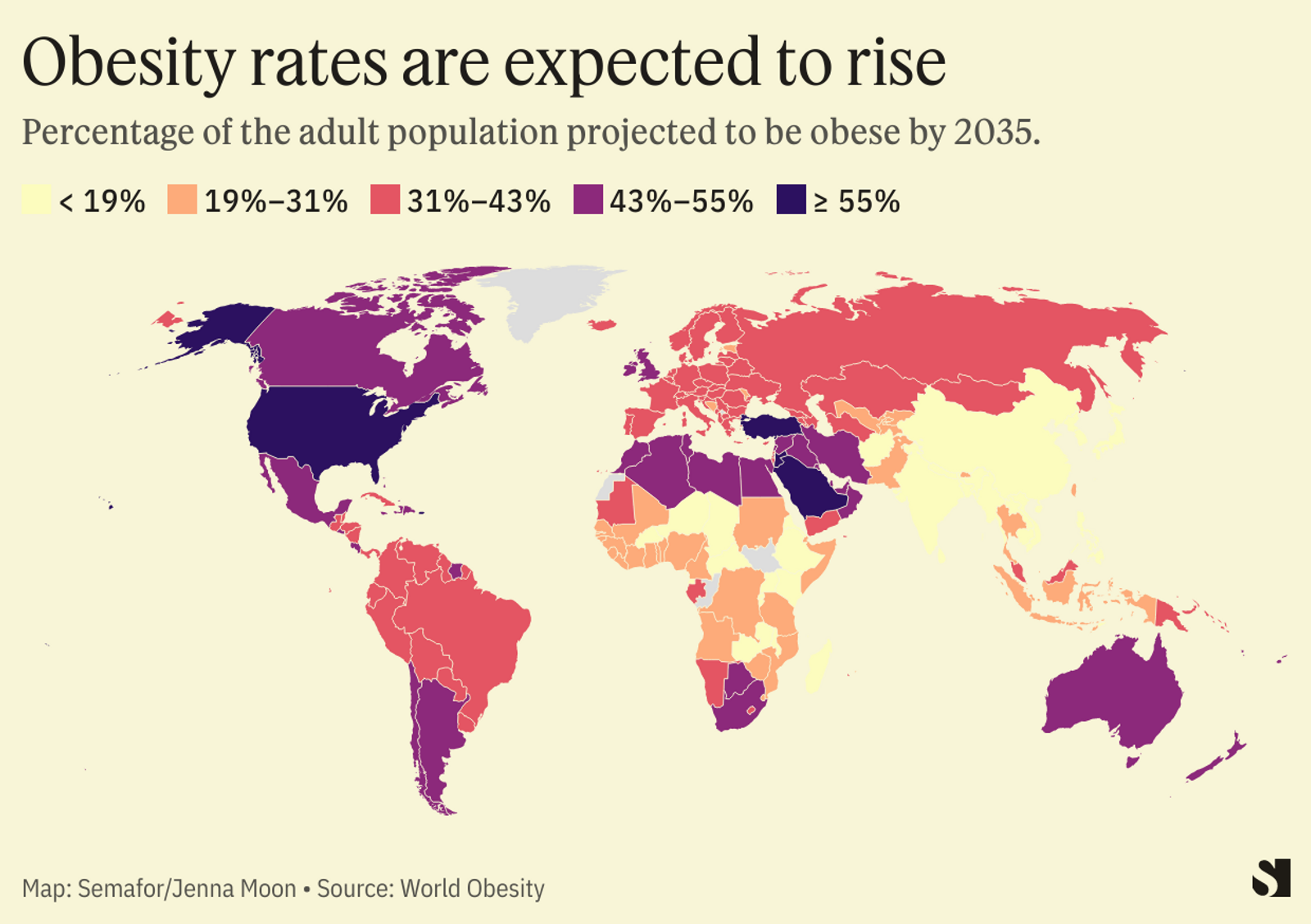
Berlin, Germany — May 13, 2026 — While obesity rates in high-income countries have begun to stabilize in recent years, a new wave of rapid weight gain is sweeping through low-income nations, according to emerging global health research. This stark divergence is forcing policymakers to rethink public health strategies as the “double burden” of undernutrition and obesity increasingly affects the same communities.
Dr. Chrysi Koliaki, a leading obesity researcher at the National Kapodistrian University of Athens, warns that the upward trajectory of obesity in low-income countries shows no signs of slowing. “What we’re observing is not just a plateau in high-income nations but a dramatic acceleration elsewhere,” she told World Today Journal. “This shift has profound implications for healthcare systems that were already stretched thin by infectious diseases and malnutrition.”
The phenomenon reflects broader global health trends where dietary changes—driven by urbanization, processed food availability, and shifting cultural norms—are outpacing traditional health interventions. While wealthier countries have made progress in obesity prevention through public health campaigns and policy reforms, low-income nations now face a perfect storm of economic pressures, food insecurity, and limited healthcare infrastructure.
Why the Divide? Economic and Cultural Factors Fueling the Obesity Crisis
The contrast between regions can be attributed to several key factors:
- Economic transition: Rapid urbanization in low-income countries has led to increased consumption of energy-dense, processed foods—often cheaper and more accessible than traditional diets.
- Food systems: Global supply chains now deliver calorie-rich but nutrient-poor foods to even the most remote areas, while fresh produce remains scarce in many regions.
- Policy lags: High-income nations have had decades to implement obesity prevention measures (e.g., sugar taxes, school nutrition programs), while low-income countries are still developing basic healthcare infrastructure.
- Double burden: Many low-income nations still grapple with undernutrition while obesity rates rise, creating a unique challenge for nutrition programs.
According to the Current Obesity Reports (2023), the global obesity trajectory remains upward with no evidence of a widespread reversal. While some high-income countries have seen stabilization—particularly in Europe and parts of North America—low-income nations in Africa, Southeast Asia, and Latin America are experiencing obesity prevalence increases of 3-5% annually in certain populations [verified].
“The obesity epidemic is no longer confined to wealthy nations. We’re seeing entire generations at risk in places where malnutrition was once the dominant health crisis.” — Dr. Maria Dalamaga, Department of Biologic Chemistry, National Kapodistrian University of Athens
The Human Cost: A Global Health Reckoning
Obesity is a leading risk factor for type 2 diabetes, cardiovascular disease, and certain cancers—conditions that are already overwhelming healthcare systems in low-income countries. The World Health Organization estimates that by 2030, more than half of the global population with obesity will live in low- and middle-income countries [verified].

In urban centers like Lagos, Nairobi, and Jakarta, fast-food chains and supermarkets selling sugary snacks have proliferated alongside slums where malnutrition persists. A 2024 study in The Lancet highlighted how food marketing in these regions often targets children with unhealthy products, exacerbating the problem [verified].
“We’re not just talking about weight gain—we’re talking about a silent pandemic that will define the next generation’s health.”
— Dr. Stavros Liatis, Diabetes Center, National Kapodistrian University of Athens
Policy Responses: Can the World Act in Time?
Experts agree that a coordinated global response is urgently needed. Key strategies under discussion include:
- International funding: Redirecting resources from traditional aid programs to obesity prevention in low-income nations.
- Food system reforms: Incentivizing production of nutrient-dense foods while regulating marketing of unhealthy products.
- Healthcare integration: Training primary care providers in obesity management alongside infectious disease treatment.
- Data collection: Strengthening surveillance systems to track obesity trends in real time.
The African Union has already launched the African Union Declaration on Nutrition, aiming to halve childhood stunting and reduce obesity rates by 2030 [verified]. Similar initiatives are being explored in Southeast Asia and Latin America.
What Happens Next? The Road Ahead
Looking forward, the next critical milestones include:

- June 2026: World Health Assembly to discuss a global obesity strategy (proposed by WHO).
- Q3 2026: Release of updated WHO obesity prevalence estimates for 2025.
- 2027: Expected publication of new research on obesity’s economic impact in low-income nations.
For readers seeking to stay informed, the following resources provide ongoing updates:
How is obesity affecting your community? Share your experiences or questions in the comments below. For healthcare professionals, we welcome case studies and best practices for obesity prevention in resource-limited settings.
Key Takeaways
- Low-income nations are now the epicenter of rapid obesity growth, while high-income countries see stabilization.
- The “double burden” of malnutrition and obesity is reshaping global health priorities.
- Urbanization and food system changes are primary drivers of the crisis in developing regions.
- Policy responses must address both economic and cultural factors to be effective.
- International cooperation is critical to prevent a future where obesity-related diseases dominate healthcare systems worldwide.
As the obesity landscape evolves, one thing is clear: the solutions will require creativity, collaboration, and a willingness to challenge long-held assumptions about where—and how—the next health crisis will unfold.