The relationship between nutrition and metabolic health has long been a cornerstone of internal medicine, but recent analysis continues to refine our understanding of how specific nutrients trigger or prevent chronic illness. Among the most critical factors is the impact of dietary fatty acids on type 2 diabetes, a complex condition where the body either resists the effects of insulin or fails to produce enough of it to maintain normal glucose levels.
Type 2 diabetes is fundamentally a multifactorial disease. It arises from a sophisticated interaction between polygenetic predispositions and environmental triggers. While the finish result is consistently hyperglycemia—excessive sugar in the bloodstream—the pathways leading to this state vary significantly depending on a patient’s genetic makeup and lifestyle choices, particularly their dietary intake of fats.
Understanding the nuance of fatty acids is essential because not all fats affect the body in the same way. While some can exacerbate metabolic dysfunction, others may offer a protective shield, potentially counteracting the damage caused by more harmful lipids. This balance is central to reducing the risk of developing metabolic diseases and managing the condition once it manifests.
The Role of Fatty Acids in Metabolic Risk
Research into dietary lipids highlights a stark contrast between different types of fatty acids. For instance, palmitic acid is associated with adverse effects that can contribute to the development of metabolic instability. However, certain other fatty acids may act as a counterbalance to these negative impacts.
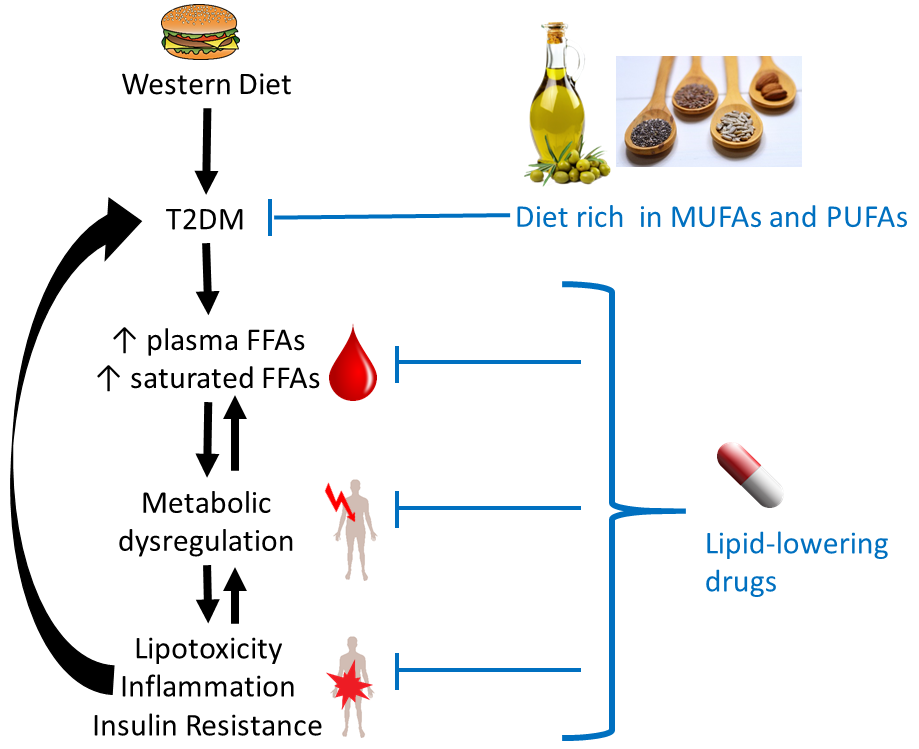
Specifically, diets rich in monounsaturated fats are consistently linked to a lower risk of developing type 2 diabetes and other related metabolic disorders. What we have is why dietary patterns such as the Mediterranean diet, which emphasizes these healthy fats, are frequently recommended by health professionals to mitigate risk Analizan el impacto de los principales ácidos grasos de la dieta en el desarrollo de la diabetes mellitus tipo 2.
The Pathophysiology of Type 2 Diabetes
To understand why dietary fats matter, one must look at the underlying mechanisms of the disease. The development of type 2 diabetes is generally driven by two primary factors: insulin resistance (where the body’s cells do not respond properly to insulin) and the deficient secretion of insulin by the pancreas Diabetes tipo 2 – Fisiopatologia.
Insulin Resistance and Hyperglycemia
Insulin resistance is often the result of several intersecting biological failures. Key contributors include:

- Inflammation: Chronic low-grade inflammation can interfere with insulin signaling.
- Obesity: Excess adipose tissue is closely linked to the development of resistance.
- Mitochondrial Dysfunction: When the “powerhouses” of the cell fail to function efficiently, it disrupts glucose metabolism.
When these factors combine, the body struggles to move glucose from the blood into the cells. This is further complicated by the overproduction of glucose by the liver (hepatic glucose production), which pushes blood sugar levels even higher, leading to sustained hyperglycemia.
Deficient Insulin Secretion
While some patients struggle with how their body uses insulin, others suffer from a failure in production. A notable factor in the deficiency of insulin secretion is the accumulation of amylin deposits, which can impair the pancreas’s ability to release insulin effectively Diabetes tipo 2 – Fisiopatologia.
Recognizing Clinical Manifestations
As hyperglycemia persists, the body exhibits several distinct clinical signs. These manifestations are the direct result of the body attempting to manage excessive blood glucose levels:
- Polyuria: Excessive urination as the kidneys attempt to flush out excess glucose.
- Polydipsia: Excessive thirst resulting from the fluid loss caused by polyuria.
- Polyphagia: Increased hunger because cells are not receiving the glucose they need for energy.
- Weight Loss: Occurs when the body begins burning fat and muscle for energy since it cannot utilize glucose.
- Vision Changes: Blurred vision is a common early sign of glucose-related ocular stress.
- Paresthesia: Tingling or numbness, often in the extremities, indicating nerve involvement.
- Acanthosis Nigricans: Darkened, velvety patches of skin, typically in folds, which serves as a physical marker of insulin resistance.
Clinical Management and the Importance of Timing
The management of type 2 diabetes requires a comprehensive approach focused on controlling associated comorbidities. This care is typically spearheaded by primary care specialists who monitor the patient’s overall metabolic health Diabetes Mellitus tipo 2 Archives.

A critical component of successful therapy is the timing of intervention. Medical evidence suggests that to reach therapeutic goals and prevent long-term complications, it is essential not to delay the process of insulinization when indicated by the patient’s clinical progression Diabetes Mellitus tipo 2 Archives.
Key Takeaways for Metabolic Health
| Factor | Impact/Effect | Role in Diabetes |
|---|---|---|
| Palmitic Acid | Adverse metabolic effects | Increases risk/exacerbates dysfunction |
| Monounsaturated Fats | Protective effects | Associated with lower risk |
| Insulin Resistance | Inefficient glucose uptake | Primary driver of hyperglycemia |
| Amylin Deposits | Impaired insulin release | Causes deficient insulin secretion |
The ongoing study of how dietary fatty acids influence metabolic pathways underscores the importance of personalized nutrition. By replacing harmful fats with monounsaturated options and recognizing the early signs of insulin resistance, individuals and providers can better manage the trajectory of this multifactorial disease.
Patients are encouraged to consult their primary care provider to establish a tailored management plan and discuss the appropriate timing for insulinization based on their specific health markers.
We invite readers to share their experiences with metabolic health management or ask questions in the comments below.