Managing shoulder injuries often presents a challenging crossroads for patients: continuing conservative therapy that may not be sufficient or opting for invasive surgery. For those dealing with partial rotator cuff tears, a regenerative approach known as Platelet-Rich Plasma (PRP) injection is gaining traction as a viable alternative to leisurely the progression of the injury and promote natural healing.
The core of this treatment lies in the body’s own biological resources. By concentrating the healing factors found in a patient’s blood, PRP therapy aims to stimulate the repair of damaged tendons and ligaments, potentially preventing a partial tear from evolving into a complete rupture. This regenerative strategy is particularly relevant for chronic pain in the shoulders, elbows, and knees, where blood circulation is often poor, making natural recovery difficult.
As an internal medicine specialist and health journalist, I have seen the evolution of regenerative medicine move from experimental stages to recognized clinical applications. In South Korea, for instance, the Ministry of Health and Welfare has recognized PRP treatment as a new medical technology, validating its use for treating damaged ligaments and tendons via Bando Orthopedic Hospital.
Understanding PRP: The Science of Self-Healing
Platelet-Rich Plasma (PRP) injection is a therapeutic procedure that involves separating the plasma from a patient’s own blood and injecting it back into a damaged area of the body. To understand why this works, one must look at the components of human blood. Plasma contains platelets, which are cells primarily known for clotting blood, but they likewise carry a variety of proteins and growth factors that induce cell growth and promote the healing of damaged tissues according to Seoul National University Hospital.
In a standard PRP procedure, the concentration of these platelets is significantly increased. When this high-concentration plasma is injected into a site of injury—such as a partially torn rotator cuff—it releases dozens of powerful growth factors. These factors act as signals to the body to mobilize its own healing resources, effectively stimulating the regeneration of damaged cartilage, tendons, and ligaments via Bando Orthopedic Hospital.
This “autologous” nature of the treatment—meaning it uses the patient’s own blood—significantly reduces the risk of allergic reactions or immune rejection, making it a safer alternative for many patients compared to synthetic grafts or foreign biological agents.
The Clinical Process: From Blood Draw to Injection
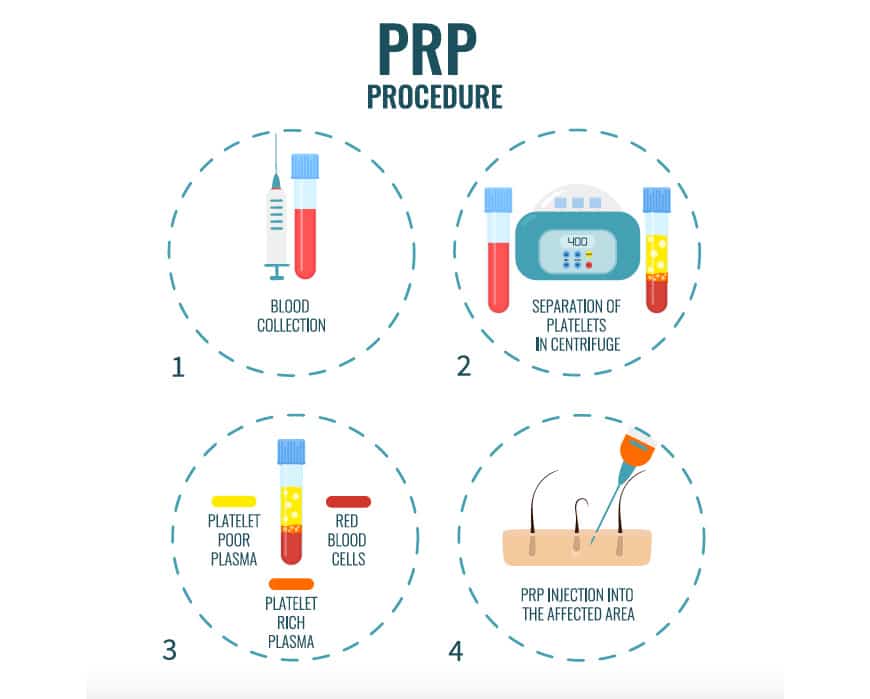
The administration of PRP therapy follows a precise medical protocol to ensure the concentration of platelets is sufficient for a therapeutic effect. The process generally involves four primary steps:

- Blood Collection: A tiny amount of the patient’s blood is drawn. The exact volume can vary depending on the target area of the body being treated via Seoul National University Hospital.
- Centrifugation: The collected blood is placed in a centrifuge and spun for approximately 10 to 15 minutes. This process separates the blood into different layers based on density via Seoul National University Hospital.
- Extraction: The platelet-rich plasma layer is carefully isolated and prepared in a syringe, removing the rest of the blood components via Bando Orthopedic Hospital.
- Precision Injection: The concentrated PRP is injected into the damaged tissue. To ensure accuracy, clinicians often use ultrasound guidance to target the specific area of the tear via Bando Orthopedic Hospital. In some cases, a local anesthetic may be administered first to reduce pain during the procedure via Seoul National University Hospital.
Essential Patient Preparations
Before undergoing PRP therapy, It’s critical for patients to review their current medications with their healthcare provider. Certain drugs, specifically antiplatelet agents or anticoagulants (blood thinners), can increase the risk of bleeding and may need to be discontinued temporarily to ensure the procedure’s safety and efficacy via Seoul National University Hospital.
Why PRP is Effective for Rotator Cuff Partial Tears
The rotator cuff consists of tendons that connect muscles to the shoulder bone. These tissues are notoriously difficult to heal because they have a limited blood supply. When a partial tear occurs, the lack of blood flow often prevents the body from repairing the gap, which can lead to the tear widening over time and eventually becoming a complete rupture.
PRP therapy addresses this specific biological limitation. By delivering a concentrated dose of growth factors directly into the tendon, the treatment bypasses the poor natural circulation of the area. This induces a “self-healing” response, encouraging the body to regenerate the damaged tissue and strengthening the remaining tendon fibers via Bando Orthopedic Hospital.
For patients, this means a potential reduction in chronic pain and a decrease in the likelihood of needing surgical intervention. By slowing the progression of a partial tear, PRP provides a window for conservative management and physical therapy to be more effective.
Comparison of PRP and Traditional Treatments
| Feature | PRP Therapy | Conventional Steroid Injections | Surgical Repair |
|---|---|---|---|
| Primary Goal | Tissue regeneration and healing | Inflammation and pain reduction | Mechanical repair of the tear |
| Source | Patient’s own blood (Autologous) | Synthetic corticosteroid | Surgical sutures/grafts |
| Recovery Time | Moderate (depends on regeneration) | Fast (temporary relief) | Long (requires extensive rehab) |
| Impact on Tissue | Promotes tissue growth | Can weaken tendons if overused | Physically reattaches tendon |
Key Takeaways for Patients
- Regenerative Potential: PRP uses concentrated platelets from your own blood to stimulate the healing of damaged ligaments and tendons.
- Targeted Application: It is particularly effective for chronic pain in areas with poor blood supply, such as the shoulder, elbow, and knee.
- Safety Profile: Because it is autologous, the risk of rejection or allergic reaction is minimal.
- Preventative Value: For partial rotator cuff tears, the goal is to slow the progression toward a complete rupture.
- Medical Oversight: Patients must disclose all medications, especially blood thinners, before the procedure.
As regenerative medicine continues to advance, the focus is shifting from merely managing symptoms to addressing the root cause of tissue degradation. Whereas not every patient is a candidate for PRP, it represents a significant step forward in non-surgical orthopedic care.
Patients interested in these treatments should consult with a board-certified orthopedic specialist to determine if their specific injury is suitable for PRP therapy. Further updates on the clinical efficacy and expanded indications for regenerative injections are expected as more long-term data becomes available from medical institutions.
Do you have experience with regenerative therapies or questions about shoulder health? Share your thoughts in the comments below or share this article with someone who may find it helpful.