A case involving a man in his 30s who delayed treatment for syphilis and subsequently developed widespread systemic symptoms and vision problems has drawn renewed attention to the dangers of untreated sexually transmitted infections. While the original report originated from a Korean medical news outlet, the clinical progression described aligns with well-documented stages of syphilis infection as outlined by global health authorities.
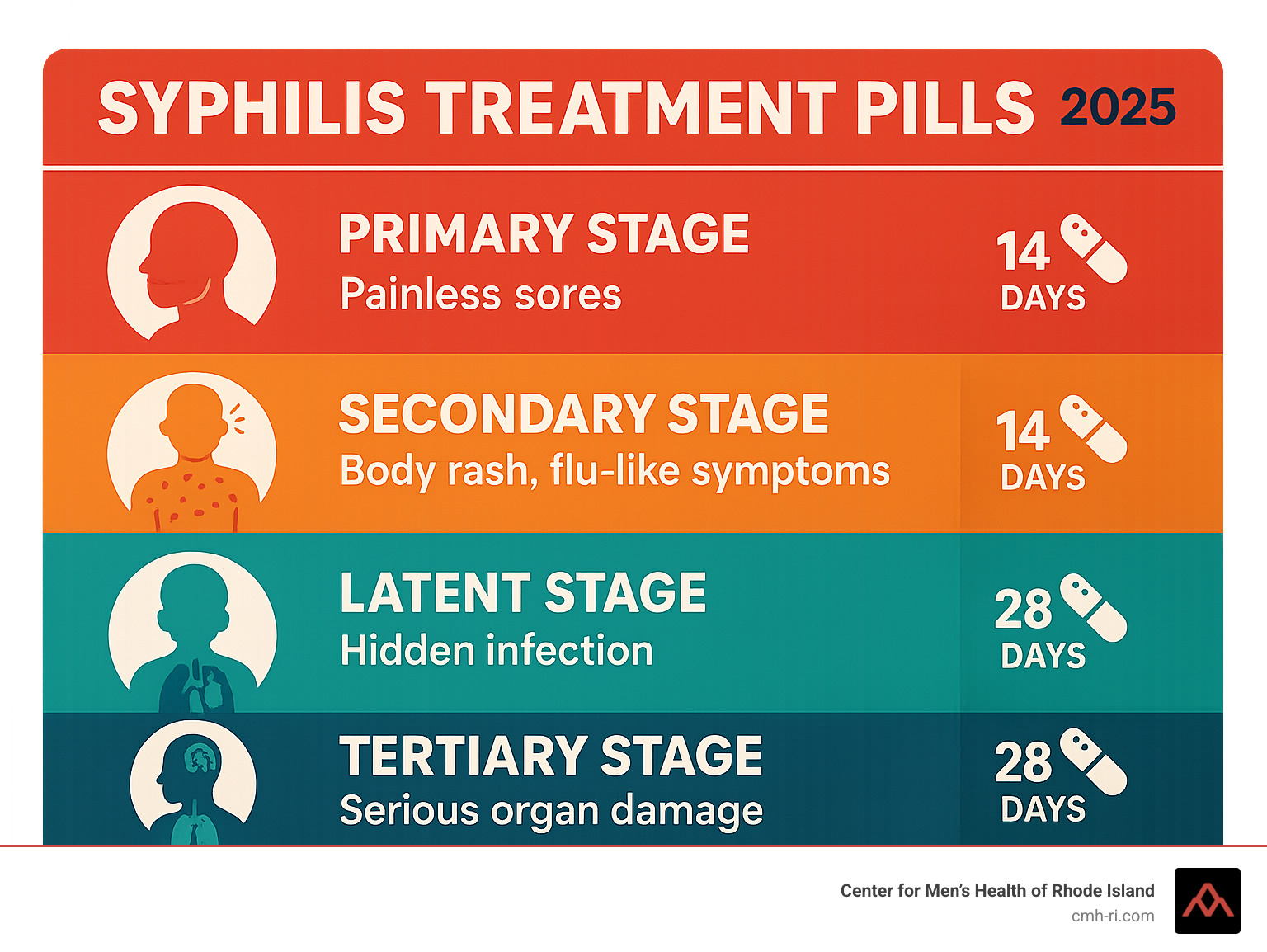
Syphilis, caused by the bacterium Treponema pallidum, progresses through distinct stages if left untreated. The initial stage often presents as a painless sore, or chancre, at the site of infection. If unnoticed or ignored, the infection advances to secondary syphilis, which can manifest with a rash, fever, swollen lymph nodes, and other flu-like symptoms. Without intervention, the disease may enter a latent phase, during which no symptoms are present but the bacteria remain active in the body. Years later, approximately 15 to 30 percent of untreated individuals develop tertiary syphilis, which can cause severe damage to the heart, brain, nerves, eyes, and other organs.
According to verified public health data, syphilis has seen a significant resurgence in recent years across multiple continents. In South Korea, the Korea Disease Control and Prevention Agency (KDCA) reported that the number of domestic syphilis cases reached 2,786 in 2024 — the highest figure since the current reporting system was established. This represents a 2.7-fold increase compared to 2014, when 1,015 cases were recorded. Of the 2024 total, approximately 93 cases were linked to overseas infection, accounting for about 3.3 percent. The KDCA too noted that syphilis was reclassified from a Class IV to a Class III infectious disease in response to the rising trend, mandating comprehensive surveillance rather than sample-based monitoring.
This upward trend is not isolated to South Korea. Similar increases have been observed in the United States, Japan, and various European nations. The U.S. Centers for Disease Control and Prevention (CDC) reported that primary and secondary syphilis cases in the United States reached their highest levels in over 70 years in 2022, with more than 200,000 cases of all stages combined. Public health officials in these regions have cited factors such as decreased condom employ, shifts in sexual networking patterns linked to dating apps, and reduced access to sexual health services during and after the COVID-19 pandemic as contributing drivers.
Neurosyphilis and ocular syphilis are recognized complications that can occur when the bacterium invades the central nervous system or eyes, respectively. Ocular syphilis may present with symptoms such as blurred vision, floaters, sensitivity to light, or even vision loss, and can resemble other inflammatory eye conditions, making diagnosis challenging without specific testing. Neurosyphilis can lead to headaches, altered mental status, stroke-like symptoms, or cranial nerve palsies. Both conditions require prompt intravenous penicillin therapy, which remains the gold standard for treating late-stage or neurological manifestations of syphilis.
The importance of early detection and treatment cannot be overstated. Syphilis is highly treatable in its early stages with a single intramuscular dose of benzathine penicillin G. For late latent syphilis or cases involving neurological or ocular involvement, a longer course of intravenous penicillin is typically required. Following treatment, patients undergo periodic blood tests (such as the rapid plasma reagin or RPR test) to ensure the infection has been fully cleared. Sexual partners should also be notified, tested, and treated to prevent reinfection and further transmission.
Public health agencies continue to emphasize routine screening for sexually active individuals, particularly those with multiple partners or who engage in high-risk behaviors. The KDCA recommends annual STI screening for sexually active adults under 30 and more frequent testing for those at increased risk. In the United States, the CDC advises syphilis screening for all pregnant women, men who have sex with men (MSM), and individuals living with HIV, among other groups.
As global syphilis rates continue to rise, health experts stress the need for increased awareness, accessible testing, and timely medical intervention. Untreated syphilis is not merely a personal health risk — it poses broader public health concerns, including the potential for congenital transmission from mother to child, which can result in stillbirth, neonatal death, or severe lifelong complications in infants.
For the most current guidance on syphilis prevention, testing, and treatment, individuals are encouraged to consult official resources from their national public health authority or trusted international organizations such as the World Health Organization (WHO).
Stay informed, prioritize your sexual health, and seek medical advice promptly if you notice any unusual symptoms — early action can prevent serious, long-term consequences.