In the northern Spanish town of Aranda de Duero, a scientific outreach event scheduled for this coming Monday will focus on the differential diagnosis of complex chronic conditions, including fibromyalgia, myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), and long COVID. Organizers say the session aims to bring together patients, healthcare providers, and researchers to explore overlapping symptoms and emerging biological markers that may help distinguish these often-confused illnesses.
The event, described as a scientific dissemination day, will address biological markers in fibromyalgia, ME/CFS, and persistent COVID, along with various research directions aimed at improving diagnostic clarity. While specific details about the venue, organizing body, or speaker lineup were not confirmed in publicly available sources, the focus on biomarker research reflects growing scientific interest in identifying objective measures for conditions historically diagnosed by symptom exclusion.
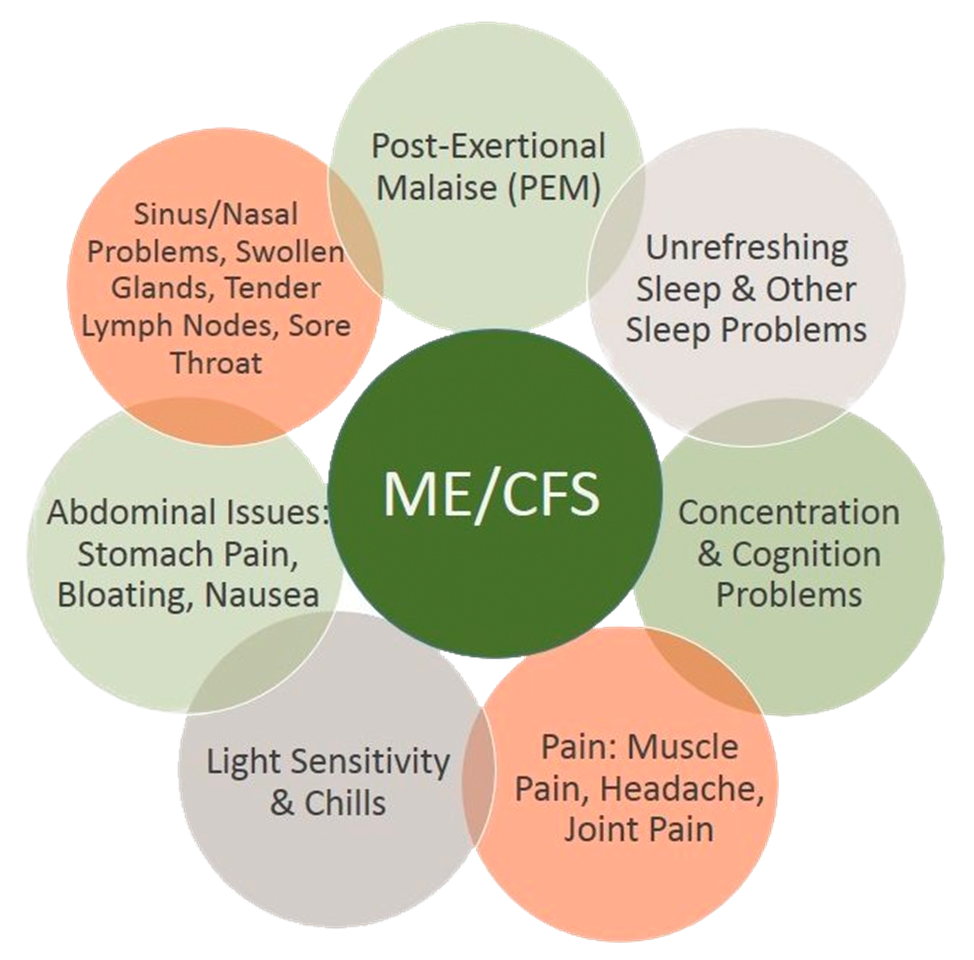
Myalgic encephalomyelitis/chronic fatigue syndrome, often abbreviated as ME/CFS, is a debilitating disorder characterized by profound fatigue, post-exertional malaise, cognitive difficulties, and autonomic dysfunction. According to the U.S. Centers for Disease Control and Prevention (CDC), the condition affects an estimated 836,000 to 2.5 million Americans, though many remain undiagnosed due to lack of awareness and standardized testing. The CDC notes that while the exact cause is unknown, factors such as immune dysfunction, metabolic abnormalities, and neurological changes are under active investigation.
Similarly, fibromyalgia involves widespread musculoskeletal pain, fatigue, sleep disturbances, and heightened sensitivity to pain. Research suggests central nervous system dysregulation may amplify pain signals, though no single biomarker has been universally accepted for diagnosis. Long COVID, or post-acute sequelae of SARS-CoV-2 infection (PASC), encompasses a range of symptoms persisting weeks or months after acute illness, including fatigue, shortness of breath, cognitive impairment, and orthostatic intolerance—many of which overlap with ME/CFS, and fibromyalgia.
Scientists have increasingly pointed to shared pathophysiological pathways among these conditions, such as autonomic dysfunction, small fiber neuropathy, mitochondrial impairment, and chronic inflammation. Studies have identified potential biomarkers including elevated inflammatory cytokines, autoantibodies against autonomic receptors, and altered metabolite profiles in metabolomic analyses. Although, none have yet been validated for routine clinical use.
The emphasis on differential diagnosis is clinically significant. Misdiagnosis or delayed diagnosis can lead to inappropriate treatments, patient frustration, and worsening outcomes. For example, graded exercise therapy—once commonly recommended for ME/CFS—has been shown in some studies to exacerbate symptoms, underscoring the need for accurate identification. Similarly, recognizing long COVID as a distinct entity with possible overlap helps guide rehabilitation and symptom management strategies.
Patient advocacy groups have long called for greater biomedical research into these conditions, arguing that psychosocial explanations have historically overshadowed biological investigations. In recent years, increased funding from institutions like the National Institutes of Health (NIH) in the United States has supported large-scale studies such as the RECOVER initiative, which aims to understand the long-term effects of COVID-19, including its overlap with ME/CFS.
In Europe, collaborative efforts like the European ME/CFS Research Network aim to harmonize data collection and accelerate biomarker discovery. While no cure currently exists for any of these conditions, symptom management through pacing, pharmacological interventions for specific symptoms (e.g., sleep aids, pain modulators), and lifestyle adjustments remains the cornerstone of care.
Events like the one in Aranda de Duero play a role in bridging the gap between research and public understanding. By presenting scientific advances in accessible formats, such gatherings empower patients to engage more effectively with healthcare providers and participate in shared decision-making. They also help reduce stigma by highlighting the biological basis of symptoms often dismissed as psychosomatic.
As research progresses, the hope is that reliable biomarkers will emerge, enabling earlier diagnosis, stratification of patient subgroups, and targeted therapies. Until then, dissemination events that clarify diagnostic complexities and promote evidence-based understanding remain vital components of patient care and scientific literacy.
For updates on upcoming medical outreach events in Spain or developments in ME/CFS, fibromyalgia, and long COVID research, individuals are encouraged to consult official health agency websites, peer-reviewed journals, and reputable patient advocacy organizations.
Share your thoughts on this story in the comments below, and help spread awareness by sharing this article with others who may benefit.