For decades, the patient-physician encounter was defined by a conversation—a rhythmic exchange of symptoms, history and empathy. Today, that rhythm is frequently interrupted by the glow of a computer screen. Many clinicians now find themselves acting as data entry clerks, spending a significant portion of their day navigating complex Electronic Health Record (EHR) systems, often continuing this work long after their shifts have ended.
This phenomenon, often referred to as “pajama time,” has contributed to a systemic crisis of clinician burnout. The administrative weight of documentation does not just exhaust the provider; it creates a physical and emotional barrier between the doctor and the patient. When a physician is focused on clicking boxes and typing narratives, the essential human element of medicine—trust and active listening—can suffer.
To address this, health systems are increasingly turning to ambient artificial intelligence. Microsoft Dragon Copilot for clinical workflows represents a shift toward “ambient clinical intelligence,” a technology designed to remove the keyboard from the exam room and return the clinician’s focus to the person sitting in front of them.
As a physician and journalist, I have seen how the promise of the EHR—to streamline care and reduce errors—has often collided with the reality of cumbersome interfaces. The introduction of generative AI into this space is not merely a technical upgrade; it is a necessary intervention for the sustainability of the healthcare workforce.
The Burden of the Digital Scribe
The modern healthcare environment is plagued by documentation overload. Clinicians are required to capture exhaustive detail for billing, legal compliance, and care coordination. However, the tools used to record this information have often turn into an end in themselves, requiring hours of manual entry that compete with direct patient care.
This administrative burden is a primary driver of professional burnout. When the cognitive load of managing a software interface exceeds the capacity of the provider, the result is emotional exhaustion and a sense of reduced personal accomplishment. The irony is that the very systems designed to improve patient safety and data accessibility have, in many cases, distanced the provider from the patient.
The goal of integrating AI into these workflows is to solve what some call the “productivity paradox”: the idea that more technology in the clinic has led to less time for actual medicine. By automating the transition from a spoken conversation to a structured clinical note, health systems can potentially reclaim hours of a clinician’s day.
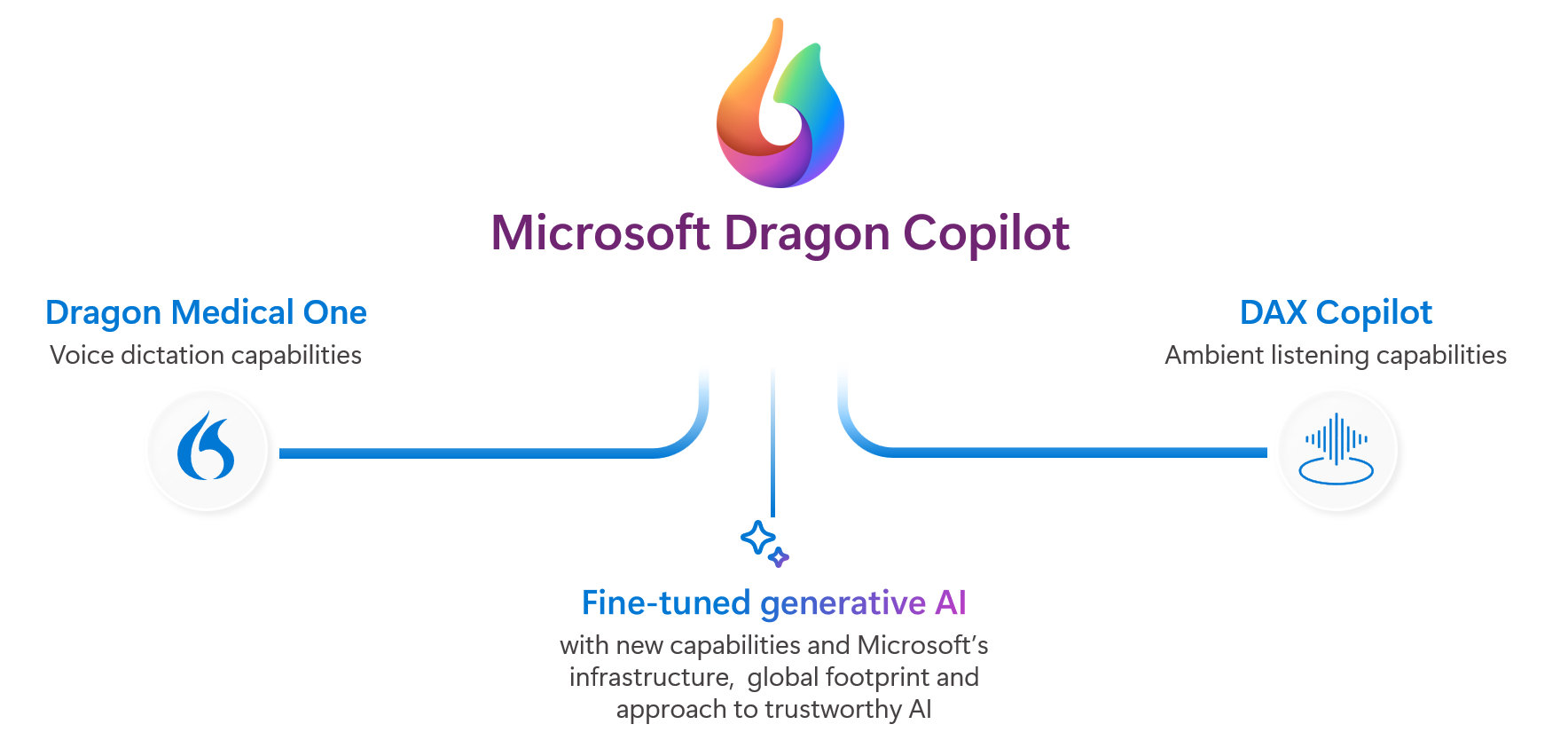
Understanding Microsoft Dragon Copilot
Microsoft Dragon Copilot, powered by Nuance’s ambient clinical intelligence, differs fundamentally from traditional medical dictation. While traditional tools required a doctor to speak into a microphone and explicitly dictate a note after the visit, ambient AI “listens” to the natural conversation between the provider and the patient in real-time.
Using advanced natural language processing and generative AI, the system identifies the clinically relevant portions of the conversation. It filters out small talk and irrelevant tangents, distilling the dialogue into a concise, structured clinical note. This draft is then presented to the physician, who reviews, edits, and signs off on the documentation, ensuring that the final record remains the responsibility of the licensed professional.
The technology is integrated into the provider’s existing workflow, often functioning as a seamless layer between the conversation and the EHR. By leveraging Microsoft Azure’s healthcare-specific AI capabilities, the system is designed to maintain strict data privacy and security standards, which are paramount in a clinical setting.
Restoring the Patient-Physician Relationship
The most immediate impact of implementing Dragon Copilot is the restoration of eye contact. When a clinician is no longer tethered to a workstation, the dynamics of the visit change. Patients report feeling more “heard,” and physicians report a renewed sense of professional satisfaction.

This shift has several downstream benefits for clinical workflows:
- Improved Data Accuracy: Because the AI captures the conversation as it happens, there is a lower risk of “recall bias,” where a physician forgets a specific detail of a visit by the time they sit down to write the note hours later.
- Reduced Cognitive Load: Clinicians can focus entirely on diagnostic reasoning and patient empathy rather than worrying about how to phrase a note for billing requirements.
- Faster Turnaround: Notes that previously took hours to complete can be finalized in minutes, reducing the backlog of unsigned charts and lowering the stress associated with administrative deadlines.
Beyond the individual visit, this technology addresses the broader issue of clinician retention. In an era of severe staffing shortages, providing tools that actively reduce the daily grind of documentation is a strategic imperative for health system leadership.
Integrating AI into Health System Workflows
For health systems looking to adopt these tools, the transition requires more than just a software installation; it requires a rethink of the clinical encounter. Integration typically involves aligning the AI tool with the organization’s specific EHR, such as Epic or Oracle Health (formerly Cerner), to ensure that the generated notes flow directly into the patient’s chart.
Implementation success generally depends on three factors:
- Physician Buy-In: Clinicians must trust that the AI is an assistant, not a replacement, and that they maintain final editorial control over the medical record.
- Workflow Optimization: Organizations must identify exactly where the “friction” exists in their current documentation process to maximize the AI’s impact.
- Governance and Compliance: Ensuring that patient consent is obtained for ambient recording and that all data handling adheres to HIPAA regulations and international privacy laws.
Many systems are starting with pilot programs in high-burnout specialties—such as primary care or emergency medicine—before scaling the technology across the entire organization. This allows them to refine the “prompting” and structuring of the notes to meet the specific needs of different medical disciplines.
Comparison: Traditional Dictation vs. Ambient AI
| Feature | Traditional Dictation | Ambient AI (Dragon Copilot) |
|---|---|---|
| Timing | Post-visit (delayed) | Real-time (concurrent) |
| Clinician Focus | Divided between patient and screen | Focused on patient |
| Effort | Manual speaking/typing | Automated drafting |
| Workflow | Linear: Visit → Dictate → Edit | Parallel: Visit/Listen → Review → Sign |
The Path Forward for Healthcare AI
The adoption of Microsoft Dragon Copilot is part of a larger trend toward “invisible” technology in medicine. The goal is for the tools to disappear into the background, leaving only the human connection. As generative AI continues to evolve, we can expect these systems to become even more nuanced, potentially helping physicians identify gaps in a patient’s history in real-time or suggesting relevant clinical guidelines based on the conversation.
However, the technology is not a panacea. AI cannot replace the clinical judgment, ethical reasoning, or emotional intelligence of a trained physician. Its value lies in its ability to handle the “clerical” side of medicine, freeing the human expert to do what they were trained to do: heal.
For health system administrators, the question is no longer whether AI will enter the clinic, but how quickly it can be deployed to save a workforce on the brink of exhaustion. The move toward ambient intelligence is a move toward a more sustainable, more human version of healthcare.
The next major milestone for many health systems will be the full integration of these AI drafts into automated billing and coding workflows, which could further reduce the administrative burden on medical staff. Official updates on these integrations are typically shared during major health IT forums and through Microsoft’s official news center.
Do you suppose AI can truly solve physician burnout, or is the problem deeper than documentation? We invite you to share your experiences with clinical AI in the comments below.