Viruses hidden in the gut may be linked to colon cancer, according to emerging research that is drawing increasing attention from scientists worldwide. While colon cancer has long been associated with genetic mutations, diet and lifestyle factors, recent studies suggest that certain viruses residing in the intestinal tract could play a role in triggering or accelerating the development of malignant tumors in the colon. This growing body of evidence points to the complex interplay between the gut microbiome, viral presence, and cellular changes that may lead to cancer.
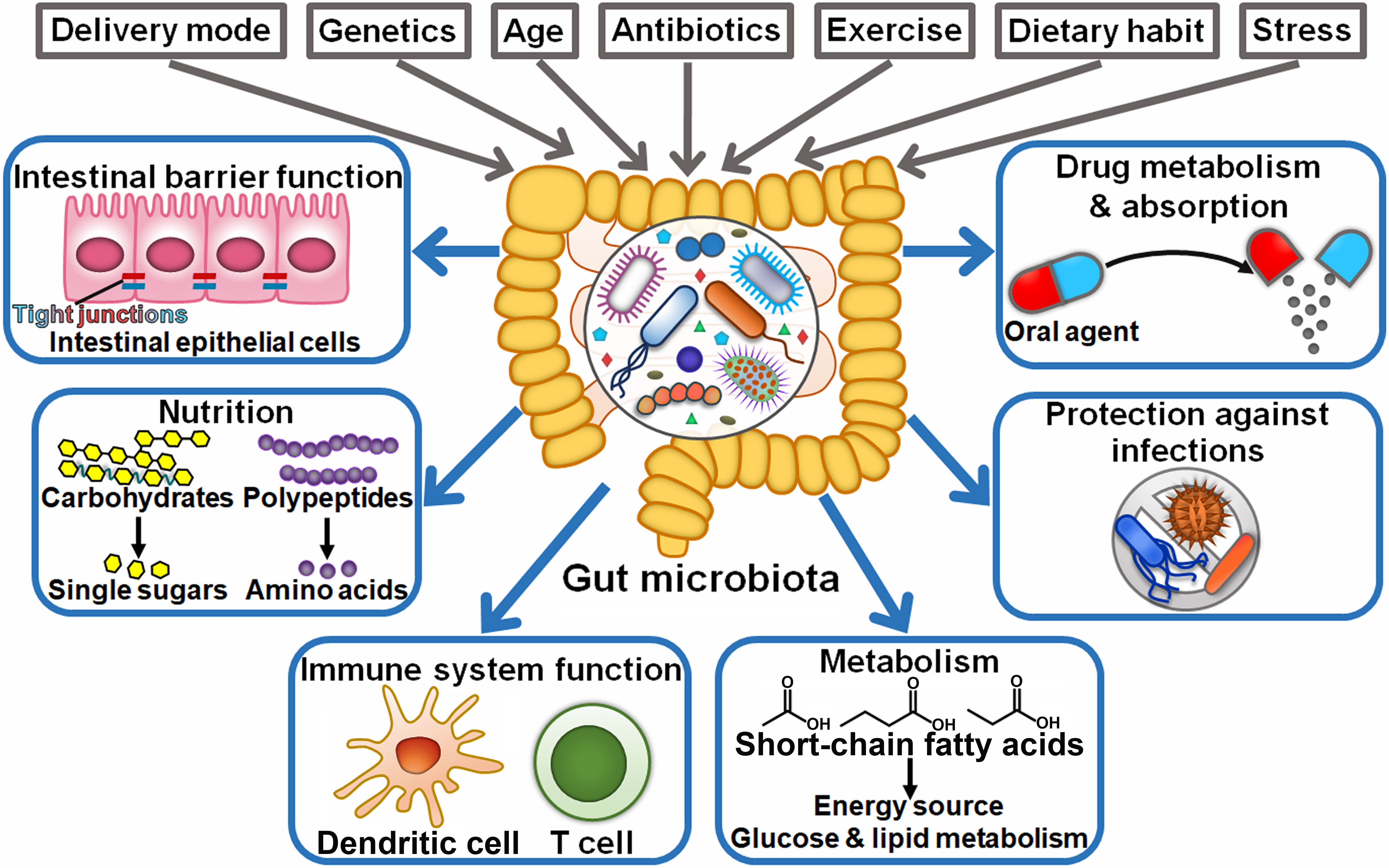
The human gastrointestinal tract hosts trillions of microorganisms, including bacteria, fungi, and viruses, collectively known as the gut microbiome. Although much research has focused on bacterial communities, scientists are now turning their attention to the virome—the collection of viruses in the gut—and its potential influence on health and disease. Some of these viruses may integrate into host cells or alter immune responses in ways that promote inflammation or DNA damage, both of which are known contributors to carcinogenesis.
One area of particular interest involves oncogenic viruses—those capable of causing cancer. While viruses like human papillomavirus (HPV) and Epstein-Barr virus (EBV) are well-established causes of cervical and certain lymphomas, respectively, researchers are investigating whether similar mechanisms could be at play in the colon. Studies have detected viral genetic material in colon tumor tissues, raising questions about whether these viruses are merely bystanders or active participants in tumor formation.
Research published in peer-reviewed journals has identified associations between specific viruses and colorectal neoplasia. For example, studies have found higher prevalence of certain polyomaviruses and herpesviruses in colorectal cancer tissues compared to healthy controls. However, scientists caution that correlation does not imply causation, and it remains unclear whether these viruses initiate cancer or simply thrive in the altered environment of a tumor.
The gut’s immune environment as well plays a critical role. Chronic inflammation, often driven by dysbiosis—an imbalance in microbial communities—has long been recognized as a risk factor for colon cancer. Viruses may contribute to this inflammatory state by infecting epithelial cells or modulating immune defenses. Some research suggests that viral activity could disrupt the intestinal barrier, allowing bacterial toxins or other harmful substances to penetrate tissue layers and trigger inflammatory cascades that damage DNA over time.
Despite these intriguing leads, experts emphasize that colon cancer remains a multifactorial disease. Established risk factors include age, family history, inflammatory bowel diseases like ulcerative colitis or Crohn’s disease, diets high in red or processed meats, obesity, smoking, and alcohol consumption. Screening methods such as colonoscopy continue to be the most effective way to detect precancerous polyps and early-stage tumors, significantly improving outcomes when cancer is found early.
Ongoing research aims to clarify the role of the gut virome in colon carcinogenesis through longitudinal studies, metagenomic sequencing, and experimental models. Scientists are analyzing stool and tissue samples from patients with and without colon cancer to identify viral signatures that might serve as biomarkers for risk or progression. While no viral vaccine or antiviral treatment for colon cancer currently exists, understanding these mechanisms could open new avenues for prevention or targeted therapies in the future.
As research evolves, public health messaging continues to stress the importance of known preventive measures: maintaining a balanced diet rich in fiber, engaging in regular physical activity, avoiding tobacco and excessive alcohol, and undergoing routine screening starting at recommended ages. For individuals with a family history of colon cancer or personal history of inflammatory bowel disease, earlier or more frequent screening may be advised based on individual risk assessment.
The exploration of viruses in the gut represents a frontier in cancer research, highlighting how deeply interconnected our internal ecosystems are with long-term health. While much remains to be discovered, the growing focus on the gut virome reflects a broader shift toward understanding cancer not just as a disease of genes, but as one shaped by the complex microbial world within us.
For the latest updates on colon cancer research and prevention guidelines, individuals are encouraged to consult authoritative sources such as the World Health Organization (WHO), the American Cancer Society, or national public health agencies. These organizations regularly review emerging evidence and provide evidence-based recommendations for screening and risk reduction.
To stay informed about developments in this field, readers can follow peer-reviewed journals in gastroenterology, oncology, and microbiology, where new findings are rigorously evaluated before being shared with the scientific community and the public.
World Today Journal remains committed to reporting on health topics with accuracy, clarity, and a commitment to scientific integrity. As new data emerges, we will continue to provide clear, verified information to facilitate readers make informed decisions about their health.
If you found this article informative, please consider sharing it with others who may benefit from understanding the latest insights into colon cancer research. Your engagement helps spread reliable health information in an era where accuracy matters more than ever.