The medical community has long viewed obesity as a complex, chronic disease rather than a failure of willpower. With the arrival of glucagon-like peptide-1 (GLP-1) receptor agonists, we have entered a transformative era of treatment. However, as a physician and journalist, I have observed that the clinical triumph of these medications is colliding head-on with the harsh realities of healthcare economics.
For many employers, particularly in the United States where health insurance is primarily company-sponsored, the surge in demand for weight-loss drugs like semaglutide and tirzepatide is creating a budgetary crisis. The tension is palpable: while these drugs offer unprecedented efficacy in reducing weight and improving metabolic health, their price tags are pushing corporate healthcare spending to a breaking point.
According to data from the Business Group on Health, a significant majority of employers are reporting that these expensive weight-loss medications are driving up their overall healthcare costs. This trend is forcing a difficult conversation among HR executives and benefits managers about who qualifies for these treatments and how to sustain coverage without bankrupting the employee health plan.
The challenge is not merely the cost of the drug itself, but the scale of the need. With obesity rates climbing globally, the pool of eligible patients is vast, and the “sticker shock” of monthly prescriptions—often exceeding $1,000 in the U.S. Market—is creating unprecedented volatility in pharmacy spend.
The Financial Friction of the GLP-1 Boom
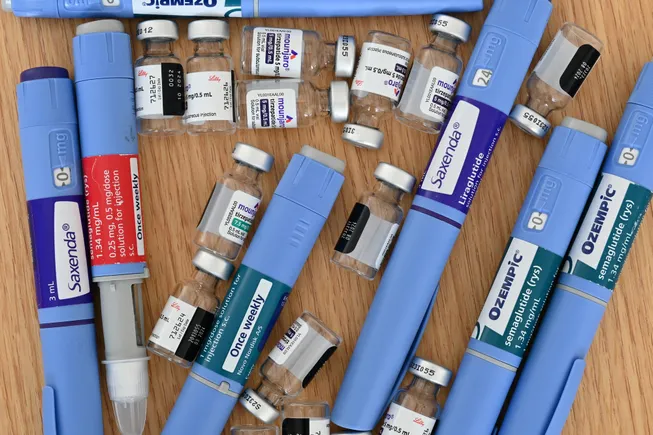
To understand why GLP-1 healthcare costs for employers are spiking, one must look at the intersection of pharmacology and pricing. GLP-1 medications, such as Wegovy (semaglutide) and Zepbound (tirzepatide), mimic hormones that target areas of the brain that regulate appetite and food intake. While the clinical results are impressive, the financial burden is shifting heavily toward the payer.
For a typical employer-sponsored plan, the cost is twofold: the high monthly acquisition cost of the medication and the administrative burden of managing a sudden influx of prescriptions. Unlike traditional medications for hypertension or high cholesterol, which are often available as low-cost generics, the most effective GLP-1s are brand-name drugs protected by patents, leaving employers with little leverage in pricing.
This financial pressure is leading to a strategic pivot in how companies approach “wellness.” For years, corporate wellness programs focused on gym memberships and step-counting challenges. Now, those programs are being overshadowed by a pharmaceutical intervention that is far more effective but exponentially more expensive. The result is a widening gap between the clinical desire to treat a patient and the corporate ability to pay for that treatment.
Clinical Value vs. Immediate Expenditure
As an MD, I must emphasize that looking at the monthly cost in a vacuum is a medical mistake. Obesity is not just about weight; it is a gateway to a constellation of expensive comorbidities, including type 2 diabetes, obstructive sleep apnea, and cardiovascular disease. The long-term “value” of GLP-1s lies in their potential to prevent these catastrophic health events.

Research published in high-authority journals has indicated that GLP-1s can significantly reduce the risk of major adverse cardiovascular events (MACE). For example, the New England Journal of Medicine has featured studies showing that semaglutide can reduce the risk of heart attack and stroke in patients with overweight or obesity and established cardiovascular disease. From a public health perspective, preventing one heart attack or one kidney failure can save a healthcare system hundreds of thousands of dollars.
However, the “ROI” (return on investment) for an employer is often delayed. A company may pay for a drug today, but the savings—in the form of fewer hospitalizations or lower disability claims—might not materialize for five or ten years. In the interim, the company may have changed employees, or the employee may have moved to a different firm. This “misalignment of incentives” is why many employers are hesitant to provide unrestricted access to these drugs, despite their clinical efficacy.
How Employers Are Managing the Cost Surge
To mitigate the impact of rising pharmacy spend, employers and their Pharmacy Benefit Managers (PBMs) are implementing several restrictive strategies. These are designed to ensure the drugs reach those who need them most while pruning “lifestyle” use from the plan.
- Strict Prior Authorization: Many plans now require a documented BMI threshold (often 30 or higher, or 27 with a comorbidity) and proof that the patient has attempted and failed traditional weight-loss interventions, such as diet and exercise.
- Step Therapy: Some insurers require patients to try older, cheaper medications first before “stepping up” to more expensive GLP-1 receptor agonists.
- Coverage Caps: A modest number of employers are exploring limits on how long a patient can remain on the drug, though this is medically controversial as GLP-1s often require long-term use to prevent weight regain.
- Value-Based Contracting: Some forward-thinking companies are negotiating contracts where the manufacturer rebates the cost if the patient does not achieve a specific percentage of weight loss.
These hurdles, while fiscally prudent for the company, can create barriers to care for the patient. When the process for obtaining a prescription becomes an administrative marathon, patients may experience delays in treatment, which can be frustrating for both the prescribing physician and the patient.
A Global Perspective on Obesity Treatment
The crisis of employer-funded costs is largely a phenomenon of the U.S. Healthcare system. In Europe, and specifically in my home city of Berlin, the approach differs because the burden falls on national health systems or statutory health insurance (Gesetzliche Krankenversicherung).
In the European Union, the European Medicines Agency (EMA) regulates approval, but individual countries negotiate prices. For instance, Germany’s AMNOG process evaluates the “added benefit” of a new drug compared to existing therapies to determine its price. Because the government has massive bargaining power, the cost to the individual and the employer is significantly lower than in the U.S. However, this often results in slower rollout or stricter eligibility criteria to ensure the sustainability of the public fund.
The global disparity highlights a fundamental question: Is obesity treatment a luxury or a fundamental right to health? When a drug can prevent a stroke or a diabetic coma, the argument for broad access becomes a moral imperative. Yet, when the cost threatens the viability of a company’s health plan, it becomes a logistical nightmare.
Key Takeaways for Employees and Employers
- For Employers: Shift the focus from “drug cost” to “total cost of care.” Analyzing the potential reduction in diabetes and heart disease costs can provide a more accurate picture of the drug’s value.
- For Employees: Be prepared to provide comprehensive clinical documentation. Ensure your physician documents your BMI and comorbid conditions clearly to navigate prior authorization hurdles.
- For Clinicians: Focus on “patient-centered” outcomes. While the cost is a barrier, the goal remains the long-term metabolic health of the patient.
What Happens Next?
The healthcare industry is currently in a state of “wait and see.” Several factors could shift the current trajectory of GLP-1 costs:

First, the pipeline of new medications is expanding. The development of oral GLP-1s (pills instead of injections) may eventually lead to lower production costs and increased competition, which typically drives prices down. Second, the U.S. Food and Drug Administration (FDA) continues to review new indications for these drugs, potentially expanding their approved use to include sleep apnea or kidney disease, which may open new avenues for insurance reimbursement.
Finally, the ongoing debate regarding PBM transparency in the U.S. May reveal how much of the “cost hike” is actually reaching the manufacturers versus how much is being captured as profit by middlemen. If pricing transparency improves, employers may find more room to negotiate sustainable rates.
The next critical checkpoint for the industry will be the release of the next annual benefits survey from the Business Group on Health, which will indicate whether the cost surge has stabilized or continued to accelerate into 2026.
Do you think obesity medications should be covered by employers regardless of cost, or should there be stricter limits to protect health plans? Share your thoughts in the comments below.