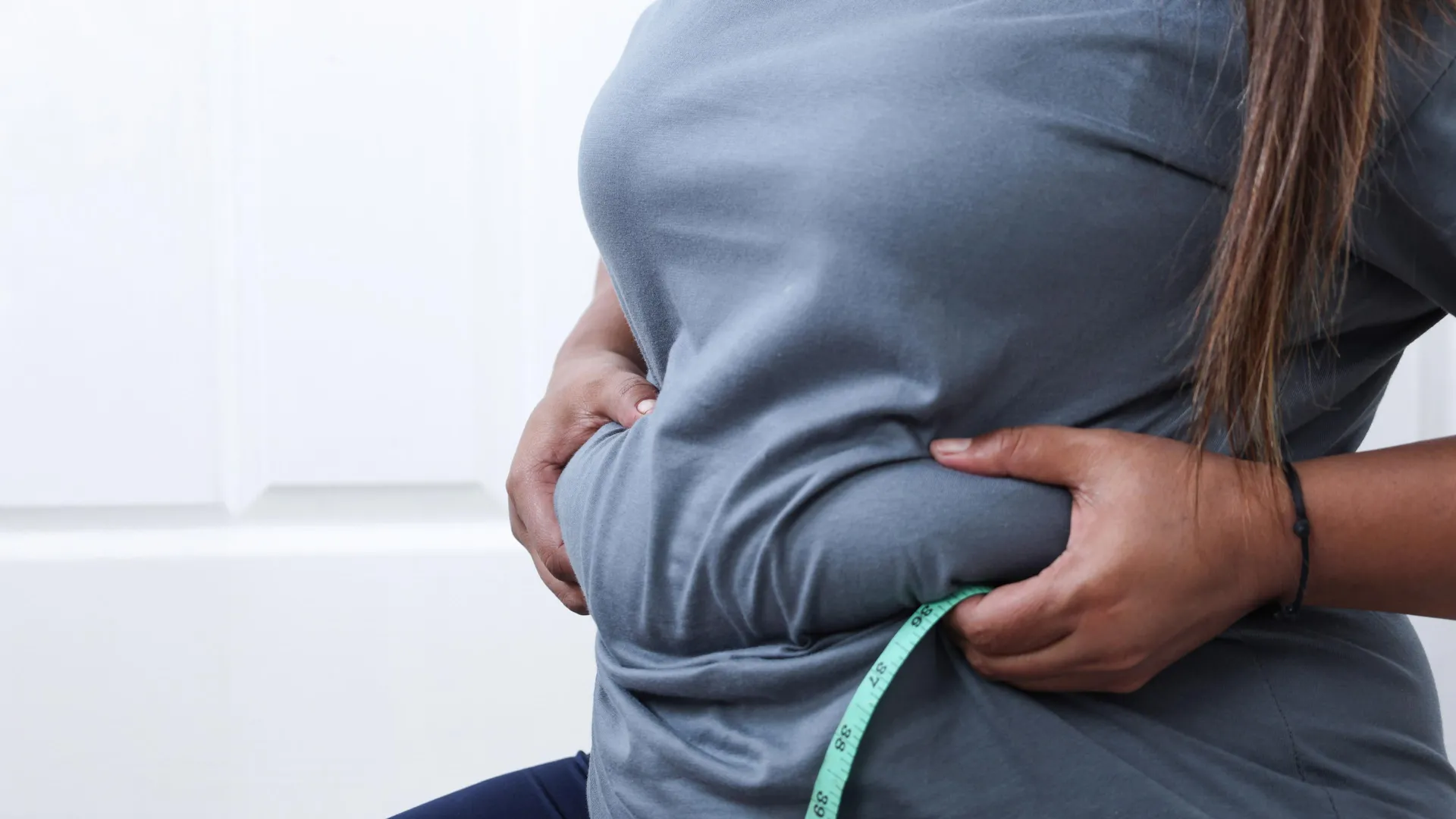
For many, the shift in body composition that accompanies aging is viewed as an inevitable part of getting older. We often talk about “middle-age spread” or the way weight seems to migrate from the hips and thighs to the abdomen. However, this redistribution is not merely a cosmetic concern; it is a significant medical transition. The accumulation of visceral fat—the deep, internal fat that wraps around vital organs—is closely linked to insulin resistance, type 2 diabetes and cardiovascular disease.
Recent research has shed new light on the hormonal drivers behind this shift, suggesting that the key to reducing visceral fat in older women may lie in a hormone often overlooked in female healthcare: testosterone. While traditionally categorized as a “male” hormone, testosterone plays a critical role in maintaining muscle mass and regulating fat distribution in women. A breakthrough study focusing on postmenopausal women recovering from hip fractures has demonstrated that a strategic combination of testosterone gel and physical exercise can effectively halt the rise of dangerous abdominal fat during a period of high vulnerability.
As a physician and journalist, I have seen how the medical community has historically underestimated the impact of androgen decline in women. We focus heavily on estrogen during menopause, but the decline of testosterone is equally impactful, contributing to sarcopenia (muscle loss) and the redistribution of adipose tissue. The findings regarding testosterone’s role in preventing visceral fat accumulation offer a promising new pathway for improving the long-term metabolic health of aging populations.
The Biological Danger of Visceral Fat
To understand why this research is so significant, we must first distinguish between the two types of fat found in the abdomen. Subcutaneous fat is the layer located directly under the skin—the fat you can pinch. While excessive subcutaneous fat can be a health concern, it is far less dangerous than visceral adipose tissue (VAT).

Visceral fat is stored deep within the abdominal cavity, surrounding the liver, pancreas, and intestines. Unlike subcutaneous fat, visceral fat is metabolically active. It acts more like an endocrine organ than a storage depot, secreting pro-inflammatory cytokines and free fatty acids directly into the portal vein, which leads straight to the liver. This process can trigger systemic inflammation and interfere with how the body processes insulin, significantly increasing the risk of metabolic syndrome. According to the Mayo Clinic, metabolic syndrome is a cluster of conditions—including increased blood pressure, high blood sugar, and excess body fat around the waist—that occur together, increasing the risk of heart disease, stroke, and type 2 diabetes.
In women, the transition through menopause triggers a sharp decline in estrogen and a gradual decrease in testosterone. This hormonal shift alters the body’s “fat mapping,” pushing the storage of lipids away from the periphery and toward the visceral compartment. For women recovering from a major trauma, such as a hip fracture, this process is often accelerated due to forced immobility and the systemic stress of injury.
The Testosterone Breakthrough in Hip Fracture Recovery
The research into testosterone’s effect on fat distribution focused on a particularly high-risk group: postmenopausal women recovering from hip fractures. A hip fracture is often a catastrophic event for an older adult, leading to a sudden decline in mobility and a rapid loss of lean muscle mass. This period of inactivity typically coincides with a spike in visceral fat accumulation, which further complicates recovery and increases the risk of secondary complications.
In the study, researchers administered a testosterone gel to a group of these women, while a control group received a placebo. Both groups were enrolled in a standardized exercise and rehabilitation program. The results were striking: the women receiving the testosterone gel experienced a significantly lower increase in visceral fat compared to those in the placebo group. More importantly, the testosterone appeared to protect lean muscle mass, providing the structural support necessary for these women to engage more effectively with their physical therapy.
This suggests that testosterone does not simply “burn fat” in a vacuum. Instead, it appears to modulate the metabolic environment, making the body more receptive to the benefits of exercise. By preventing the rapid accumulation of visceral adipose tissue during the recovery phase, the treatment may reduce the long-term cardiovascular and metabolic risks associated with hip fracture recovery.
The Synergy of Hormones and Movement
One of the most critical takeaways from this research is that the testosterone gel was not a standalone “miracle cure.” Its success was intrinsically tied to the exercise component of the recovery program. This synergy highlights a fundamental principle of endocrine health: hormones provide the biological environment, but physical activity provides the stimulus.

Testosterone promotes protein synthesis in muscle cells and inhibits the creation of new fat cells (adipogenesis) in the visceral region. When combined with resistance and aerobic exercise, this creates a powerful metabolic loop. The hormone preserves the muscle—which is the body’s primary site for glucose disposal—while the exercise burns calories and improves insulin sensitivity. Without the exercise, the potential for testosterone to reduce visceral fat is significantly diminished; without the testosterone, the ability of an older, recovering patient to build and maintain the muscle necessary for effective exercise is compromised.
This “dual-track” approach—hormonal support paired with movement—addresses the two primary challenges of aging: the loss of muscle (sarcopenia) and the gain of visceral fat (adiposity). Together, these two trends create a state known as sarcopenic obesity, which is associated with higher mortality rates and a severe loss of independence in the elderly.
Breaking the Gender Myth of Testosterone
For decades, testosterone has been viewed almost exclusively as a male hormone. In clinical practice, this bias has often led to the neglect of androgen deficiency in women. While women produce far less testosterone than men—primarily in the ovaries and adrenal glands—it is essential for bone density, cognitive function, libido, and, as this research proves, metabolic regulation.
The decline of testosterone in postmenopausal women is not just about sexual health; it is about systemic vitality. When testosterone levels drop, women lose the hormonal “brake” that prevents fat from accumulating in the abdomen. By recognizing testosterone as a vital component of women’s endocrine health, clinicians can move toward a more holistic approach to aging that goes beyond estrogen replacement therapy.
However, it is imperative to note that testosterone therapy must be handled with extreme caution and strict medical supervision. The use of androgens in women can lead to side effects such as hirsutism (excess hair growth), acne, and voice deepening if dosages are not precisely calibrated. Because testosterone can influence growth factors, its use is generally contraindicated in women with a history of certain hormone-sensitive cancers, such as breast cancer. The goal is “replacement” or “optimization” to physiological levels, not “supraphysiological” dosing.
What So for the Future of Geriatric Care
The ability to stop or slow the accumulation of visceral fat as we age has profound implications for public health. If this strategy can be scaled and safely implemented, we could see a reduction in the prevalence of metabolic syndrome among the aging population. This would not only extend life expectancy but, more importantly, extend “healthspan”—the period of life spent in decent health, free from chronic disability.

For patients recovering from major orthopedic injuries, this research suggests that the window immediately following a fracture is a critical time for metabolic intervention. Rather than focusing solely on the bone healing, the medical team can address the systemic metabolic crash that often follows. By implementing a protocol of hormonal optimization and targeted exercise, we can prevent the “metabolic slide” that often leads to a permanent loss of mobility and a decline in cardiovascular health.
Looking forward, we can expect more rigorous clinical trials to determine the ideal dosage of testosterone for different demographics of postmenopausal women and to explore whether similar results can be achieved in women who have not suffered a fracture but are struggling with age-related visceral obesity. The integration of endocrine science with geriatric rehabilitation marks a shift toward “precision aging,” where treatments are tailored to the specific hormonal profile of the patient.
Key Takeaways for Metabolic Health
- Visceral vs. Subcutaneous: Visceral fat is the dangerous internal fat surrounding organs, linked to inflammation and insulin resistance.
- The Testosterone Connection: Testosterone helps regulate fat distribution and preserve muscle in both men and women.
- The Power of Synergy: The combination of testosterone gel and exercise is more effective at reducing visceral fat than either intervention alone.
- Recovery Window: The period following a major injury, like a hip fracture, is a critical time to prevent metabolic decline.
- Medical Supervision: Hormone therapy in women requires precise dosing and screening for contraindications to avoid side effects.
The next confirmed checkpoint for this area of research will be the publication of expanded longitudinal studies tracking the long-term cardiovascular outcomes of women who received testosterone during fracture recovery. These results will determine if the reduction in visceral fat translates directly into a lower incidence of heart disease and stroke over a five-to-ten-year period.
Do you believe hormone therapy should be more widely integrated into women’s geriatric care? We invite you to share your thoughts and experiences in the comments below or share this article with others who may find this medical innovation helpful.