In Ukraine, the ongoing war has created a silent health emergency that extends far beyond the battlefield. As frontlines shift and communities face relentless disruption, people living with chronic illnesses are finding their conditions deteriorating rapidly—not due to the diseases themselves, but because the systems meant to manage them have fractured under pressure. What were once manageable conditions like diabetes, hypertension, and heart disease are now escalating into life-threatening crises, forcing patients into emergency care when routine monitoring and treatment become impossible.
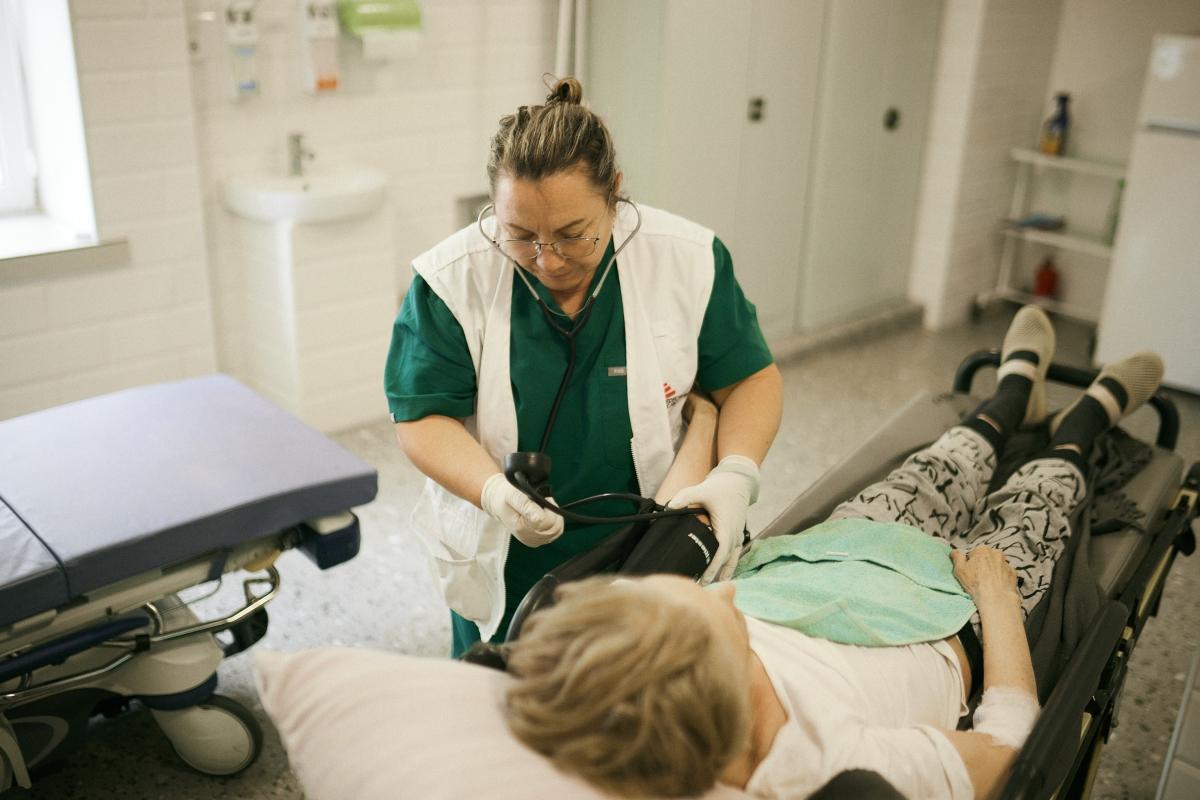
This invisible burden was highlighted in recent observations by Médecins Sans Frontières (MSF) teams operating near active conflict zones. Medical staff report a troubling pattern: patients arriving for simple check-ups are increasingly being admitted directly to hospitals due to sudden, severe complications from long-term illnesses. The organization notes that this trend disproportionately affects older adults, whose health declines quietly until a breaking point is reached—often triggered by stress, displacement, or interrupted access to medication and care.
One such case involved Vira, a 64-year-old woman from Mykolaïv who fled after Russian bombardments destroyed her home and those of her children. Now living in temporary housing in Ostrivka, she described growing weakness and blurred vision—symptoms that led her to seek help at a hospital after being unable to find a local doctor. Upon examination, MSF medical staff confirmed she was suffering from complications related to her diabetes and immediately arranged for her transfer to a specialized service capable of providing the urgent care she needed.
According to MSF data collected since the beginning of the year, more than 75 percent of patients examined by their teams in frontline-area hospitals who were living with chronic conditions required emergency referral to specialized services. Over 3,200 such patients have been assessed in these areas, underscoring the scale of unmet medical need among those managing long-term illnesses amid war.
The strain on Ukraine’s healthcare system has been compounded by repeated attacks on medical infrastructure, shortages of essential medicines, and the displacement of both patients and healthcare workers. Pharmacies have closed or been damaged, supply chains disrupted, and many clinics unable to operate consistently. For individuals relying on daily insulin, blood pressure medication, or anticoagulants, even short interruptions can have serious consequences.
Stress and trauma—ubiquitous in wartime environments—also play a significant role in worsening chronic conditions. Elevated cortisol levels from prolonged anxiety can increase blood glucose, raise blood pressure, and contribute to inflammation, all of which exacerbate underlying illnesses. Combined with poor nutrition, limited mobility, and reduced access to preventive care, these factors create a perfect storm for health deterioration.
MSF has responded by deploying mobile clinics and supporting local health facilities to stabilize patients and restore continuity of care where possible. Their efforts focus on bridging gaps in the system—providing emergency stabilization, facilitating referrals, and helping reestablish access to ongoing treatment. Still, the organization emphasizes that sustainable solutions require a functioning national health infrastructure, which remains under severe strain.
The situation reflects a broader pattern seen in prolonged conflicts: while war injuries capture global attention, the gradual decline in population health due to neglected chronic diseases often goes unnoticed until it reaches a critical stage. Unlike acute trauma, these conditions do not present with visible wounds, making them harder to track and easier to overlook in humanitarian assessments.
Addressing this hidden crisis demands more than emergency medical response. It requires sustained investment in supply chains for essential medicines, protection of healthcare facilities under international humanitarian law, and support for health workers operating under extreme conditions. Long-term planning must integrate chronic disease management into disaster response frameworks, ensuring that patients are not left behind when systems collapse.
As of now, there are no publicly announced large-scale initiatives specifically targeting chronic care continuity in Ukraine’s war-affected regions beyond existing humanitarian medical efforts. Monitoring bodies such as the World Health Organization continue to assess healthcare access in the country, but detailed, real-time data on chronic disease outcomes remain limited due to security and access challenges.
For updates on humanitarian health operations in Ukraine, including those related to chronic disease management, readers can follow official channels from Médecins Sans Frontières and the World Health Organization’s Health Emergencies Programme.
What are your thoughts on how the international community can better support non-communicable disease care in prolonged crises? Share your perspective in the comments below, and help spread awareness by sharing this article with others who may not realize the full scope of health impacts in war zones.