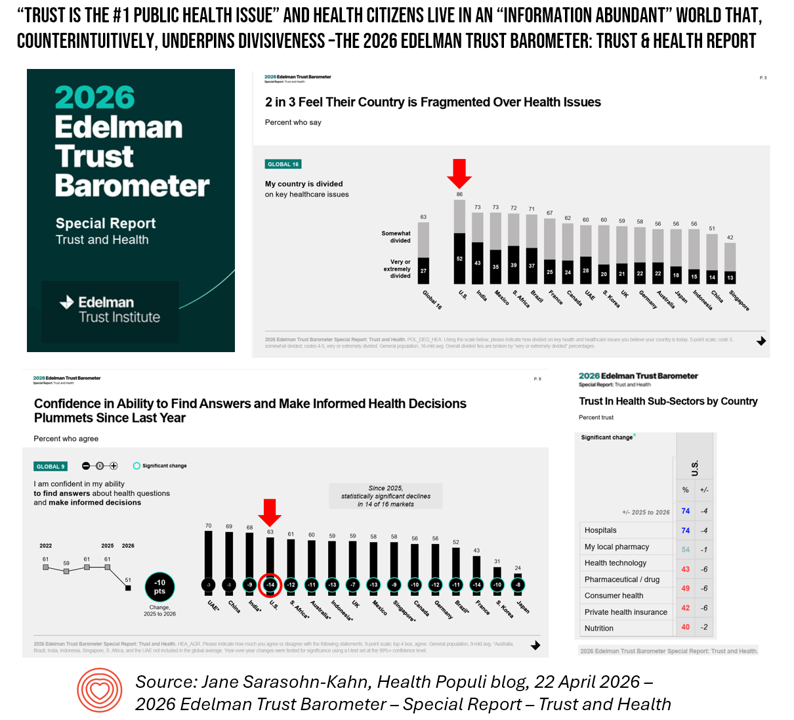
In an era where health information is more accessible than ever, a paradox has emerged: despite unprecedented access to data, many people feel less confident in making health decisions. This contradiction lies at the heart of the 2026 Edelman Trust Barometer’s special report on health, which identifies declining trust as the foremost challenge facing global public health today.
The report, released in April 2026 following its debut at the World Economic Forum in January, reveals that confidence in personal health decision-making has dropped significantly in several countries. In the United States, the share of people who felt confident in their ability to discover accurate health information and create informed choices fell by 14 percentage points from 2025 to 2026 — the steepest decline among all nations surveyed, matched only by France.
This erosion of confidence occurs even as individuals report consuming more health information than before. Rather than fostering clarity, the abundance of sources — ranging from social media and artificial intelligence to peer networks and celebrity influencers — has contributed to confusion and polarization. Trust — not disease outbreaks, vaccine hesitancy, or nutrition gaps — has become the central barrier to effective public health action worldwide.
According to the Edelman Trust Institute, which conducted the global survey, trust is no longer primarily shaped by institutional authority but by proximity and relatability. People are increasingly turning to local figures — such as pharmacists, community health workers, faith leaders, and doulas — for guidance, often placing equal or greater trust in them than in national health agencies or government officials.
This shift reflects a broader evolution in how trust is built and maintained. Over the past five years, the narrative has moved from polarization during the pandemic to a growing sense of isolation — what Edelman terms the “Age of Insularity.” In this environment, individuals curate their own information ecosystems, seeking validation from like-minded sources rather than engaging in broad, evidence-based dialogue.
Despite these challenges, certain actors remain consistently trusted. Globally, “my doctor” remains the most trusted source of health information, with 80% of respondents expressing confidence in their physician’s guidance. Medical scientists follow closely at 73%, while trust in friends and family stands at 64%. In contrast, only 61% of global respondents said they trust major health authorities such as the World Health Organization or the United Nations.
Meanwhile, novel players are gaining influence in specific domains. Artificial intelligence, in particular, is reshaping how people approach health decisions. The report notes that two-thirds of individuals who use AI fluently say they are able to perform at least one health-related task as well or better than a doctor — whether interpreting symptoms, researching treatment options, or managing chronic conditions.
This growing reliance on AI and non-traditional sources is especially pronounced in preventive health. While doctors remain the go-to for diagnosis and acute treatment, many people now turn to peers, influencers, and algorithm-driven platforms for advice on nutrition, supplements, and lifestyle changes. Edelman describes this area — prevention — as “the most competitive clinical domain,” where traditional clinicians face increasing competition for attention and trust.
The abundance of information has not led to consensus. On the contrary, the report finds that 70% of global respondents believe at least one of six commonly debated health claims, ranging from the safety of water fluoridation to the role of vaccines in population control. Notably, those who hold the most polarized views are also the most active seekers of information, consulting a wider array of sources in search of validation.
This behavior underscores a key insight: in an environment of information overload, formal credentials are no longer the sole determinant of trust. Instead, perceived empathy, shared experience, and accessibility often carry more weight than degrees or institutional affiliations. As one expert noted during the report’s launch panel, “People just seek you to care about them — that is the best credential you can bring.”
The panel, hosted by the Edelman Trust Institute and featuring leaders from public health, technology, and pharmaceutical sectors, emphasized practical steps for rebuilding trust. Dr. Megan Ranney, Dean of the Yale School of Public Health, stressed that trust is built in small, consistent moments — not grand gestures. She advocated for training clinicians in active listening and creating space for patients to share what they’ve learned outside the clinic without feeling dismissed.
Dr. Uché Blackstock, founder of Advancing Health Equity, echoed this, noting that when patients bring self-sourced information to appointments, This proves often not a challenge to authority but a reflection of systemic gaps in access, time, and connection. Clinicians who acknowledge these realities — rather than reacting defensively — are better positioned to foster collaboration.
From a systems perspective, Sreejit Mohan of Sanofi argued that divisiveness does not lead to disengagement but can actually stimulate deeper engagement — if met with the right approach. He urged health organizations to shift from one-way communication to dialogue, inviting communities to co-create solutions rather than simply receive information.
Dr. Garth Graham, who leads healthcare and public health initiatives at Google/YouTube, highlighted the importance of tone and respect. Drawing on a lesson from his mother — “hearing is one thing, listening is another” — he emphasized that effective communication requires genuine engagement, not just the dissemination of facts. In an age of algorithmic curation, he argued, the human element — showing up, listening, and responding with care — remains irreplaceable.
The consensus among experts was clear: rebuilding trust requires a shift from centralized authority to distributed, community-based engagement. This “All of Society” approach calls for clinicians, scientists, technologists, creators, and local leaders to perform together — not as competing voices, but as coordinated partners in public understanding.
Practical steps include training community health workers to serve as trusted intermediaries, integrating pharmacists and faith-based counselors into public health outreach, and designing digital tools that prioritize clarity and context over virality. Crucially, any effort must begin with listening — not assuming what people necessitate, but asking them directly.
As the 2026 Edelman Trust Barometer makes clear, the future of public health does not depend solely on new treatments or technologies. It depends on whether people believe the system is working for them — and whether they feel seen, heard, and respected in their journey toward better health.
For ongoing updates on global trust in health institutions and emerging trends in health communication, readers can refer to the Edelman Trust Institute’s annual reports and the World Health Organization’s publications on health literacy and community engagement.
We welcome your thoughts: How has your trust in health information sources changed in recent years? What sources do you find most reliable, and why? Share your experiences in the comments below to help foster a broader conversation about trust, access, and the future of public health.