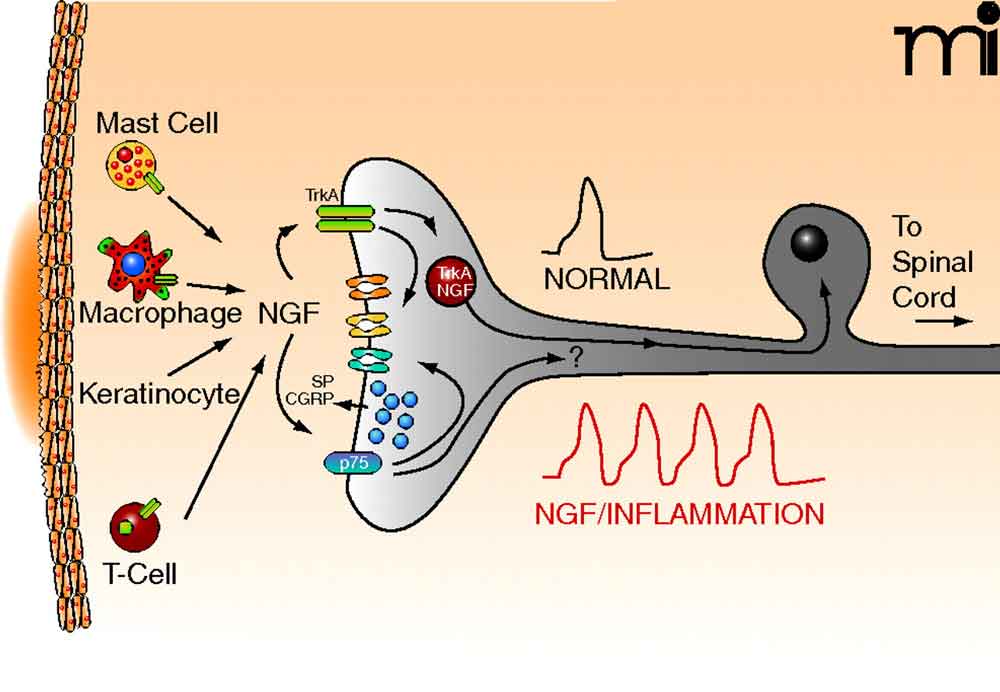
For years, medical science has viewed nerve growth factor (NGF) primarily as a messenger of pain. In the context of osteoarthritis, NGF is known to increase within affected joints, contributing to the chronic discomfort that millions of people experience. However, novel research suggests that this protein does far more than simply signal pain to the brain; it may actually drive the structural degradation of the joint itself.
A study published in Arthritis & Rheumatology reveals that nerve growth factor and osteoarthritis share a deeper relationship than previously understood. Researchers found that NGF alone is sufficient to trigger several pathological features typical of osteoarthritis in healthy joints, suggesting that the protein plays a critical role in the disease’s pathogenesis.
The findings challenge the traditional understanding of osteoarthritis as a disease primarily driven by “wear and tear” or cartilage loss. By demonstrating that a single protein can induce joint swelling and bone changes in healthy subjects, the study opens new avenues for understanding how the nervous system interacts with joint tissues to accelerate disease progression.
Inducing Osteoarthritis-Like Changes in Healthy Joints
To investigate the biological effects of NGF, a research team led by Alia M. Obeidat conducted experiments using naïve murine knee joints. The study utilized 10 to 15-week-old male wildtype C57BL/6 mice to see if the introduction of NGF could mimic the symptoms of osteoarthritis without any prior joint injury or degradation.
The researchers administered repeated intra-articular (IA) injections of either 50 ng or 500 ng of NGF, or a vehicle control, twice a week over a period of four weeks. The results showed a clear dose-dependent response. Mice receiving the NGF injections experienced significant increases in knee swelling and knee hyperalgesia (increased sensitivity to pain) compared to the control group.
Beyond the immediate symptoms of pain and swelling, the researchers observed significant structural alterations. The injections led to increased bone mineral density in the medial subchondral bone and the development of medial pre-osteophytes—bony projections that typically form along joint margins in osteoarthritis patients. Interestingly, despite these significant pathological changes, the researchers noted that there was no overt cartilage damage, highlighting that NGF can trigger joint pathology even before the cartilage begins to break down.
The Role of Nociceptors and Joint Innervation
One of the most significant discoveries of the study involves how NGF alters the innervation of the joint. The researchers used NaV1.8-tdTomato reporter mice to track the behavior of nociceptors, the sensory neurons responsible for detecting painful stimuli.
The data revealed that NGF caused increased sprouting of nociceptors within the medial synovium. This physical change in the joint’s nerve structure was not random; it was preceded by the upregulation of axonal growth pathways in the dorsal root ganglia (DRGs). By performing bulk RNA sequencing on the DRGs after three injections, the team confirmed that the nervous system was being primed for this growth before the physical sprouting occurred in the knee.
This process suggests a cycle where NGF not only makes existing nerves more sensitive but actively recruits and grows new nerve endings into the joint tissue, potentially creating a feedback loop that sustains and amplifies pain and inflammation.
Uncovering the Cellular Mechanism via scRNAseq
To understand exactly which cells were driving these changes, the team employed single-cell RNA sequencing (scRNAseq) of the synovium. This high-resolution technique allowed them to see how individual cells responded to the presence of NGF.
The sequencing revealed a significant upregulation of genes associated with three primary pathological processes: neuronal sprouting, synovial fibrosis and ossification. The study identified lining fibroblasts as playing a key role in these changes. These cells, which normally line the joint capsule, appeared to be central to the structural remodeling of the joint in response to NGF.
By linking the activity of lining fibroblasts to the physical changes in bone density and nerve growth, the research provides a more comprehensive map of how a chemical signal (NGF) translates into a physical deformity (osteophytes and fibrosis) within the joint.
Key Takeaways from the NGF Study
- Structural Impact: NGF can cause knee swelling, synovial pathology, and increased bone mineral density in the medial subchondral bone.
- Nerve Sprouting: The protein triggers the growth of new nociceptors in the synovium, driven by pathways in the dorsal root ganglia.
- Cartilage Preservation: Pathological changes occurred without overt cartilage damage, suggesting NGF acts early in the disease process.
- Cellular Drivers: Lining fibroblasts in the synovium are key mediators of fibrosis and ossification.
- Clinical Context: While anti-NGF antibodies have shown analgesic effects, previous clinical development was halted due to joint-related side effects.
Implications for Future Treatment
The realization that NGF is a driver of joint pathology, rather than just a symptom of pain, has significant implications for the development of future therapies. For some time, antibodies against NGF have been explored for their analgesic effects in patients with painful knee osteoarthritis. However, as noted in the PubMed abstract of the study, clinical development of these antibodies was stopped due to side effects observed in the joints.

Understanding that NGF actively remodels the joint—affecting bone density and nerve innervation—may assist researchers design more targeted interventions. Instead of simply blocking pain signals, future treatments might focus on preventing the structural “re-wiring” of the joint and the fibrosis driven by lining fibroblasts.
This study underscores the complexity of osteoarthritis, positioning it not just as a failure of cartilage, but as a systemic failure involving the nervous system, the synovial lining, and the underlying bone structure.
As researchers continue to explore the role of neurotrophins in joint health, the next step will be determining if these murine findings translate directly to human pathology and whether targeting the specific pathways in the dorsal root ganglia can prevent the onset of joint remodeling.
We welcome your thoughts on these developments in joint health. Please share this article or leave a comment below to join the conversation on medical innovation.