For many adults, the transition into their fifties marks a period of reflection on long-term health and longevity. However, one of the most significant threats to independence in later life often progresses without a single symptom until a critical failure occurs. Bone health is frequently overlooked until a fracture happens, making the strategy of preventing osteoporosis after 50 a vital priority for global public health.
Osteoporosis is a skeletal condition characterized by a decrease in bone density, which weakens the internal structure of the bone and significantly increases the likelihood of fractures. According to the MSD Manual, these fractures can occur under minimal force, through a simple fall, or in some cases, without any apparent cause at all.
Medical recommendations from the World Health Organization (WHO) and other international health bodies emphasize a shift toward early prevention rather than late-stage treatment. Because the condition is often “silent,” the focus has moved toward proactive interventions—specifically nutrition and physical activity—to maintain skeletal integrity as the body ages.
The Silent Nature of Bone Loss
One of the most dangerous aspects of osteoporosis is its lack of early warning signs. Many individuals live with declining bone density for years without knowing it. The first indication of the disease is often a broken bone, which can lead to a sudden and severe loss of mobility.
While most fractures are painful, some spinal fractures may occur without immediate pain, instead manifesting as gradual physical deformities. This asymptomatic progression makes routine screening and a commitment to preventing osteoporosis after 50 essential for those in high-risk categories.
Identifying High-Risk Populations
While osteoporosis can affect individuals of all ethnicities, certain demographic factors significantly increase vulnerability. Data from the Mayo Clinic indicates that women of White or Asian descent are at a higher risk, particularly those who have passed the age of menopause.
The biological driver behind this increased risk in women is primarily hormonal. The decline in estrogen levels following menopause reduces the body’s ability to maintain bone density. When combined with the natural effects of aging, the balance between bone resorption and bone formation shifts, leading to a net loss of bone mass.
Key Risk Factors Summary
- Age: Natural decline in bone mass occurs as people grow older.
- Hormonal Changes: A drop in estrogen levels, especially in post-menopausal women.
- Nutritional Deficits: Insufficient intake of calcium and low levels of vitamin D.
- Ethnicity: Increased prevalence among White and Asian populations.
The Pillars of Science-Backed Prevention
Preventing the onset of bone fragility requires a synergistic approach combining nutrition and lifestyle. Global health guidelines highlight three primary interventions: calcium, vitamin D, and targeted exercise.
The Synergy of Calcium and Vitamin D
Calcium is the fundamental building block of bone tissue. However, the body cannot effectively utilize calcium without sufficient levels of vitamin D. Research indicates that a deficiency in vitamin D impairs the absorption of calcium in the gut, which directly leads to a decline in bone density and a subsequent increase in fracture risk.
To combat this, medical guidance suggests a combination of dietary intake and moderate exposure to sunlight, which triggers the natural production of vitamin D in the skin. This nutritional foundation is critical for maintaining the components that preserve bone strength and density.
The Impact of Resistance Training
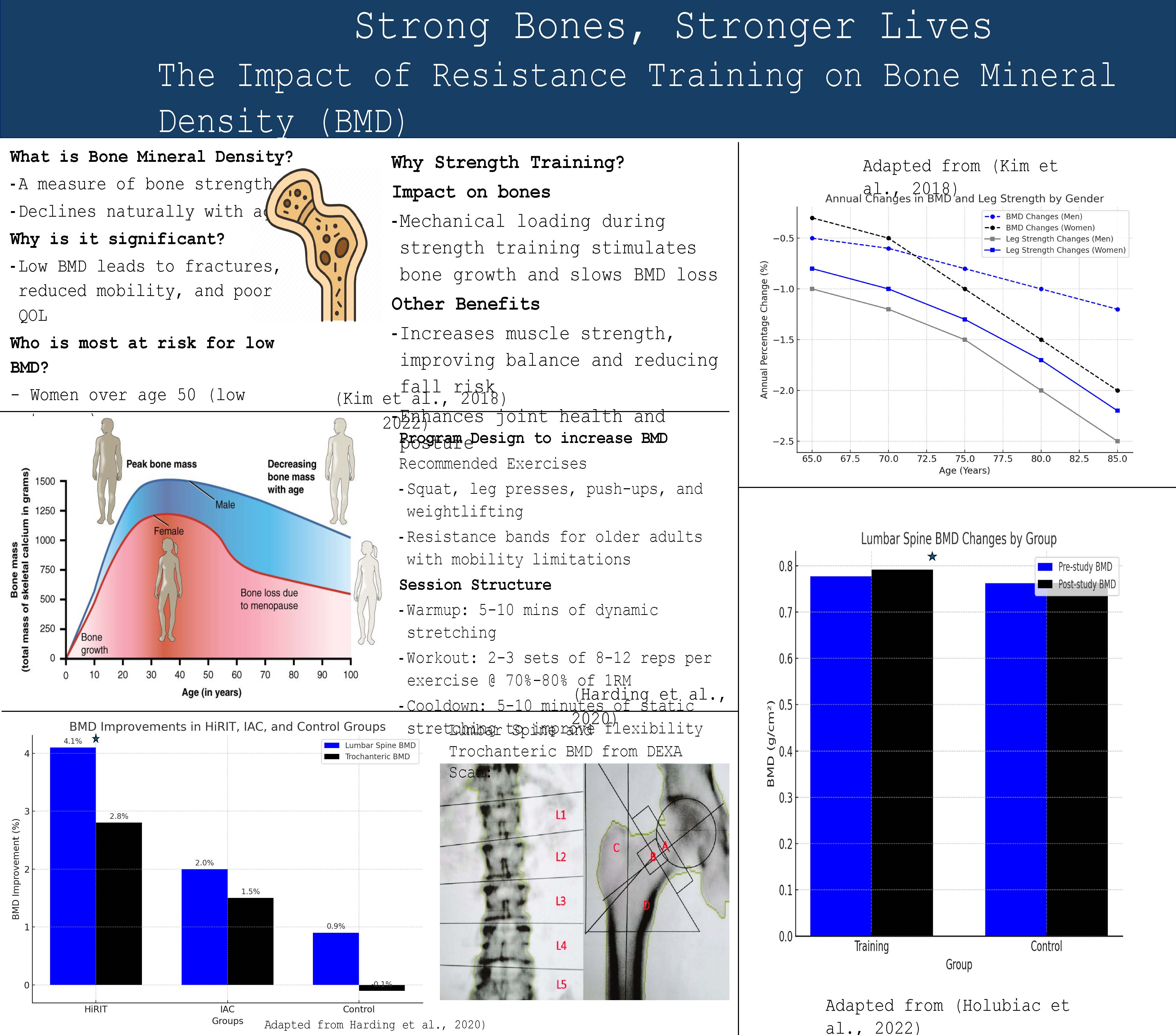
Physical activity is not merely about cardiovascular health; it is a mechanical necessity for bone maintenance. While general activity is beneficial, resistance training—exercises that challenge the muscles and bones—is particularly effective. These exercises stimulate the body to build new bone tissue and maintain existing strength, providing a structural defense against fractures.
Screening and Clinical Monitoring
Because osteoporosis is often undetectable through physical examination alone, clinical screening is the only way to accurately assess risk. Physicians use bone density scans to measure the mineral content of the bone, allowing them to categorize patients by risk level and tailor prevention or treatment plans accordingly.
Regular screenings are recommended for those over 50, especially for women post-menopause, to detect bone loss early. This allows for the implementation of preventative measures before a fracture occurs, aligning with the global healthcare trend of prioritizing early intervention over reactive treatment.
Key Takeaways for Bone Health
- Prioritize Nutrition: Ensure adequate calcium intake paired with vitamin D to maximize absorption.
- Stay Active: Incorporate resistance training to stimulate bone growth and strength.
- Sun Exposure: Get moderate sunlight to support natural vitamin D production.
- Get Screened: Schedule periodic bone density tests to monitor skeletal health.
The path forward for those over 50 involves a proactive partnership with healthcare providers. The next critical step for individuals in this age group is to consult with a physician to determine their specific bone density baseline and establish a personalized nutrition and exercise regimen. By focusing on these scientifically supported interventions, the risk of debilitating fractures can be significantly reduced.
Do you have questions about bone health or screening? Share your thoughts in the comments below or share this guide with someone who could benefit from these prevention strategies.

