Recent research has reinforced a significant understanding in oncology: intestinal metaplasia, particularly as seen in Barrett’s esophagus, serves as the sole precursor pathway to esophageal adenocarcinoma. This conclusion emerges from large-scale studies integrating epidemiological and genomic data from thousands of patients, offering clarity on a disease often diagnosed at advanced stages.
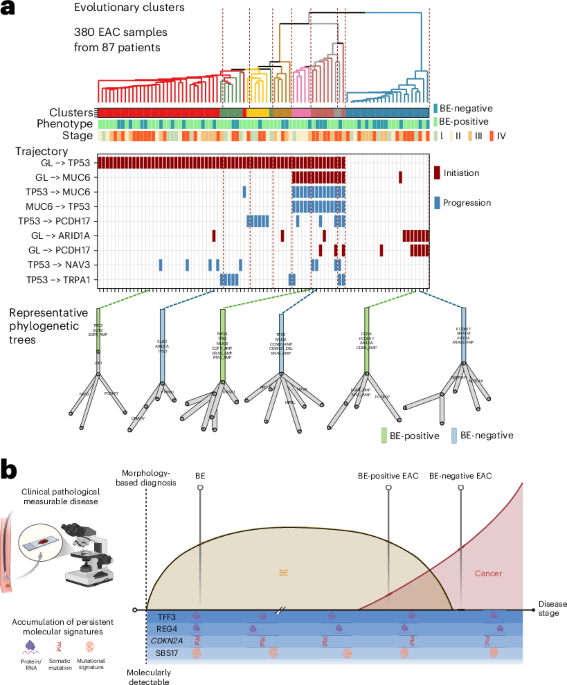
The findings, published in Nature Medicine on April 23, 2026, stem from an analysis of over 3,100 patients with esophageal adenocarcinoma. Researchers compared tumors arising in the presence and absence of detectable Barrett’s esophagus at diagnosis. Despite half of the patients showing no identifiable Barrett’s esophagus when cancer was found, molecular analysis revealed consistent signs of intestinal metaplasia across all cases.
This suggests that Barrett’s esophagus, while sometimes undetectable by standard endoscopic methods at the time of cancer diagnosis, remains the originating lesion. The study indicates that in many instances, the cancerous process may have obliterated or replaced the original Barrett’s tissue, making it invisible during examination.
Genomic profiling further supported this unified origin. Specific molecular features characteristic of early Barrett’s esophagus development were detected in both Barrett’s-positive and Barrett’s-negative esophageal adenocarcinoma tumors. Shared risk factors, evolutionary trajectories, and lineage markers tied to intestinal metaplasia were present across all tumor subtypes analyzed.
These insights carry direct implications for clinical practice. They reinforce the importance of monitoring and managing Barrett’s esophagus as a precancerous condition, even when cancer appears to arise without it. Early detection strategies targeting intestinal metaplasia could improve outcomes for a malignancy historically associated with poor survival rates.
The research underscores that esophageal adenocarcinoma follows a single pathogenic route initiated by intestinal metaplasia. Understanding this pathway may guide future screening programs and therapeutic interventions aimed at preventing malignant transformation before invasive cancer develops.
As esophageal adenocarcinoma continues to rise in prevalence globally, identifying its definitive precursor allows for more precise public health approaches. Focusing surveillance on intestinal metaplasia offers a logical step toward reducing the burden of this aggressive cancer through timely intervention.
Ongoing efforts to refine detection methods for early Barrett’s esophagus and monitor its progression remain critical. Future studies may explore how molecular markers of intestinal metaplasia can be leveraged in non-invasive screening tools to identify at-risk individuals before cancer develops.
For now, the evidence converges on one clear conclusion: intestinal metaplasia is not merely a risk factor but the essential precursor to esophageal adenocarcinoma, shaping how clinicians approach prevention and early diagnosis.