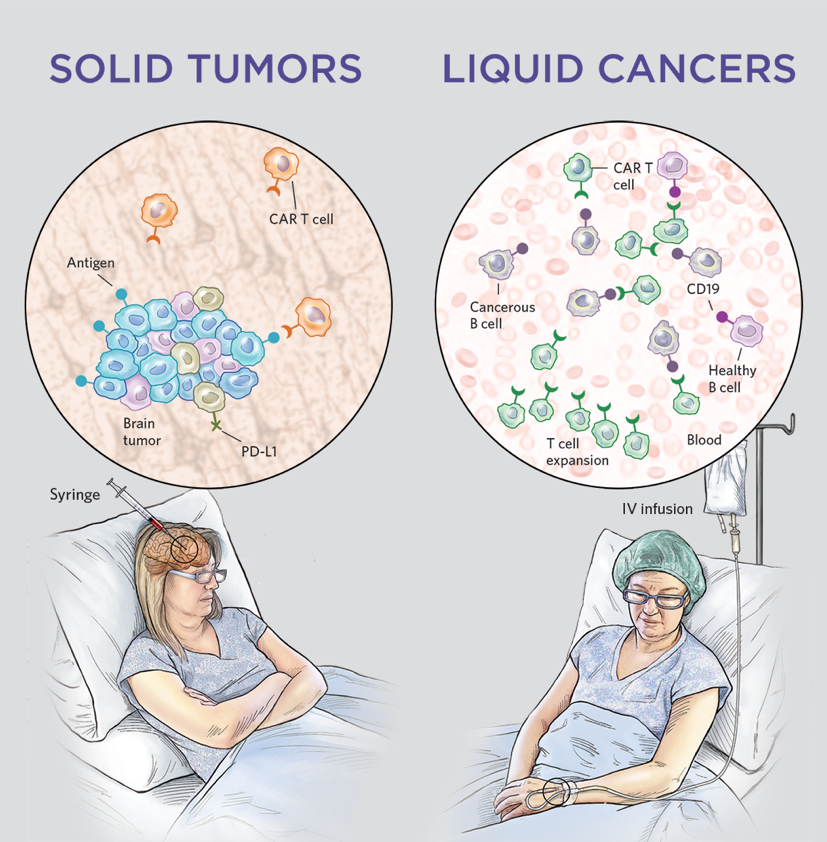
Scientists at the University of Pennsylvania have reported promising early results from a first-in-human clinical trial of a novel chimeric antigen receptor (CAR) T cell therapy designed to treat solid tumors. The treatment, known as SynKIR-110 or KIR-CAR, demonstrated safety and signs of efficacy in patients with advanced ovarian cancer, mesothelioma, and cholangiocarcinoma (bile duct cancer) during a Phase I dose-escalation study presented at the American Association for Cancer Research (AACR) Annual Meeting in San Diego in April 2026.
The findings mark the first clinical data for this innovative approach, which engineers T cells to mimic natural killer (NK) cell receptors in order to overcome a major barrier in immunotherapy: T cell exhaustion. Unlike conventional CAR T cells that remain continuously active and can become depleted over time, the KIR-CAR design incorporates a multi-chain structure that allows the receptor to assemble only when it encounters its target antigen, creating an intrinsic “on-off” mechanism that promotes periods of rest between activations.
“This represents exciting because we’re seeing good efficacy signals, even at low doses, and limited toxicity in cancer types that have never had an approved cell therapy,” said Janos L. Tanyi, MD, PhD, principal investigator of the multicenter STAR-101 Phase 1 Clinical Trial and associate professor of Obstetrics and Gynecology at the Perelman School of Medicine, University of Pennsylvania. Tanyi presented the results during a Clinical Trials Plenary Session at the AACR meeting, where he emphasized the potential for improved persistence and reduced side effects compared to existing CAR T approaches.
The trial enrolled nine patients with advanced solid tumors who had progressed despite prior treatments. As dose levels increased, researchers observed a corresponding rise in anti-tumor activity, suggesting a dose-dependent response. Importantly, the therapy appeared well-tolerated, with no dose-limiting toxicities reported in the initial cohort—a significant consideration given the history of severe side effects associated with some CAR T cell therapies in hematologic malignancies.
Carl June, MD, a pioneer in CAR T cell therapy and the Richard W. Vague Professor in Immunotherapy at Penn, noted during the meeting’s opening plenary that translating success from blood cancers to solid tumors has long been hampered by the immunosuppressive tumor microenvironment and the tendency of engineered T cells to become dysfunctional. The KIR-CAR strategy represents one of several emerging approaches aimed at addressing these limitations by mimicking the natural biology of NK cells, which are known for their ability to respond dynamically to threats without becoming chronically activated.
According to the research team, SynKIR-110 is engineered to recognize a specific tumor-associated antigen, though the exact target was not disclosed in the public presentation. The therapy’s design separates antigen recognition from T cell activation across multiple polypeptide chains, requiring both components to come together upon tumor engagement to trigger signaling. This structural feature is intended to prevent tonic signaling—a key driver of exhaustion—by allowing the receptor to disassemble and reset after each encounter.
Outside experts have cautioned that while early-phase trials like this one are critical for establishing safety and biological activity, larger studies will be needed to determine whether the observed antitumor effects translate into meaningful clinical benefits such as tumor shrinkage or prolonged survival. The research team confirmed that enrollment and dose escalation are ongoing, with plans to expand to additional cohorts and monitor long-term T cell persistence and tumor responses.
The AACR Annual Meeting, held annually and recognized as one of the foremost gatherings in oncology research, provided a platform for the Penn team to share these preliminary findings with the global scientific community. As of the presentation date in April 2026, no regulatory filings or published peer-reviewed results from the STAR-101 trial had been made publicly available beyond the conference abstract (CT104).
Moving forward, investigators will continue to evaluate biomarker correlates of response, including immune profiling and serial imaging, to better understand which patients are most likely to benefit. The trial remains active at multiple sites across the United States, though specific locations were not detailed in the public disclosures.
For patients and families affected by hard-to-treat solid tumors, the development of next-generation cellular immunotherapies like KIR-CAR offers a cautious but meaningful signal of progress. While it remains too early to declare a breakthrough, the emphasis on reducing exhaustion and improving safety profiles reflects a evolving direction in the field—one that prioritizes not just potency, but sustainability of the immune response.
Those interested in following the trial’s progress can consult ClinicalTrials.gov using the identifier NCT04887432, which corresponds to the STAR-101 study titled “A Phase 1 Study of SynKIR-110 in Subjects With Relapsed or Refractory Solid Tumors.” The listing confirms the study’s status as active but not recruiting as of the most recent update, though this may change as the trial advances through its phases.
As research into engineered cell therapies continues to evolve, approaches that integrate principles from innate immunity—such as NK-inspired CAR designs—may play an increasingly important role in expanding the reach of immunotherapy beyond blood cancers into the complex landscape of solid tumors.
We invite readers to share their thoughts and experiences in the comments below. If you found this information useful, please consider sharing it with others who may benefit from learning about emerging advances in cancer treatment.