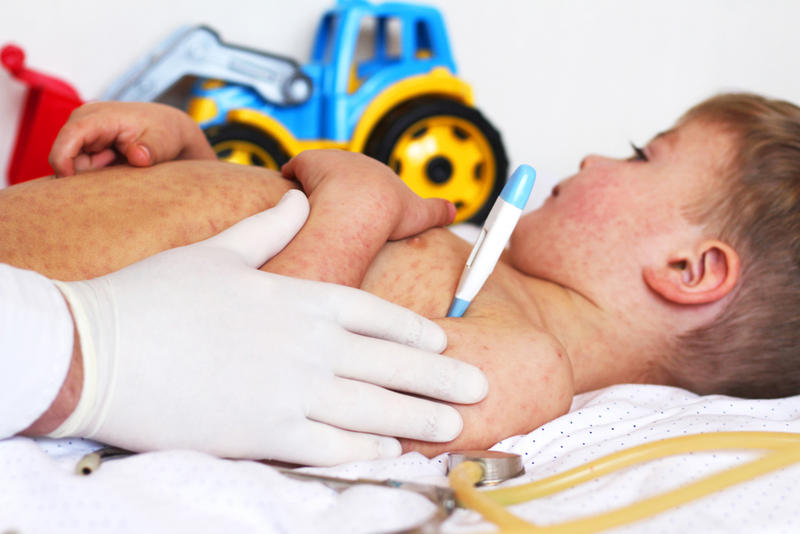
For decades, the medical community has operated under a singular, absolute truth regarding measles: the only way to stop the virus is to prevent it. Since the introduction of the first vaccine in 1963, our strategy has been one of total defense. We do not treat measles; we avoid it. However, a significant scientific shift is underway as researchers identify neutralizing antibodies that could finally provide a targeted treatment for those already infected.
This development comes at a critical juncture. Across the globe, we are witnessing a troubling resurgence of the virus, driven by gaps in vaccination coverage and a rise in vaccine hesitancy. While the vaccine remains the gold standard for public health, the lack of a therapeutic intervention has left a dangerous void for patients who cannot be vaccinated—such as infants or the severely immunocompromised—and for those who succumb to the virus despite global efforts to eradicate it.
The identification of these antibodies represents more than just a laboratory success; We see a fundamental change in how we approach one of the most contagious diseases known to man. By moving from a purely preventive model to one that includes therapeutic options, medicine is preparing for a future where a measles diagnosis is no longer a race against time and supportive care, but a condition that can be actively neutralized.
As a physician and journalist, I have seen how the “vaccination gap” creates pockets of vulnerability. When immunity drops below the critical threshold of 95%, the virus finds a foothold. The promise of a monoclonal antibody treatment offers a secondary line of defense, providing passive immunity to those who are most at risk and potentially reducing the severe complications—such as pneumonia and encephalitis—that make measles so deadly.
The Science of Neutralization: How the New Treatment Works
To understand why this discovery is a breakthrough, we must first understand how the measles virus operates. The measles virus enters human cells by binding to specific receptors, primarily using its hemagglutinin (H) protein to “unlock” the cell membrane. Once inside, the virus hijacks the cell’s machinery to replicate, spreading rapidly through the respiratory tract and eventually the entire body.
The research focuses on identifying and synthesizing neutralizing antibodies—specifically monoclonal antibodies—that can bind to the virus’s surface proteins before they reach the cell. These antibodies act as molecular shields. By coating the virus, they block the H protein from attaching to the host cell, effectively neutralizing the virus’s ability to infect new cells and halting the progression of the disease.
Unlike a vaccine, which teaches the body’s own immune system to produce antibodies over time (active immunity), these treatments provide “passive immunity.” The antibodies are produced in a laboratory and administered directly to the patient. This means the protection is instantaneous, which is vital for patients who have already been exposed to the virus or those whose immune systems are too weak to respond to a traditional vaccine.
This approach is similar to how we have successfully treated other viral threats and autoimmune conditions. By isolating the exact sequence of antibodies that are most effective at neutralizing the measles virus, scientists can now create a standardized therapy that can be scaled for global distribution.
Closing the Gap: Why Vaccines Alone Are Not Enough
It is important to be clear: the development of a treatment does not replace the need for vaccination. According to the World Health Organization (WHO), measles remains a leading cause of death among young children globally, despite the availability of a safe and effective vaccine. The goal of a therapeutic treatment is to fill the gaps where vaccines cannot reach.
There are three primary groups who would benefit most from an antibody-based treatment:
- The Immunocompromised: Patients undergoing chemotherapy, those with HIV/AIDS, or organ transplant recipients often cannot receive live-attenuated vaccines. For these individuals, a measles infection is often catastrophic.
- Infants: There is a window of vulnerability between birth and the first dose of the MMR (measles, mumps, and rubella) vaccine. Passive immunization via antibodies can provide critical protection during this period.
- The Exposed: While post-exposure prophylaxis (PEP) exists, a potent antibody treatment could be administered to those recently exposed to the virus to prevent the onset of symptoms and reduce the likelihood of transmission to others.
the global landscape of immunity is fracturing. In several regions, including parts of Eastern Europe and North America, vaccination rates have fallen below the herd immunity threshold. The Centers for Disease Control and Prevention (CDC) emphasizes that maintaining high vaccination coverage is the only way to prevent large-scale outbreaks. However, as outbreaks become more frequent, the medical necessity for a “rescue therapy” becomes undeniable.
From Laboratory to Clinic: What Happens Next?
The transition from identifying a neutralizing antibody in a lab to administering a drug in a hospital is a rigorous process. The researchers have successfully demonstrated the efficacy of these antibodies in vitro (in test tubes) and in animal models. The next critical phase involves human clinical trials to determine the optimal dosage, the duration of protection, and the safety profile of the treatment.
One of the primary challenges in developing monoclonal antibodies is the cost of production and the complexity of delivery. For a measles treatment to be truly effective on a global scale, it must be affordable and accessible in the low-income regions where the virus continues to cause the most fatalities. This will require collaboration between academic researchers, pharmaceutical companies, and international health bodies.

scientists are looking into “broadly neutralizing antibodies” (bNAbs). Because viruses can mutate, researchers want to ensure that the antibodies they develop are effective against all circulating strains of the measles virus. The goal is a “universal” treatment that remains effective regardless of the specific genetic drift of the virus in different parts of the world.
If clinical trials prove successful, this treatment could be integrated into emergency response protocols. During a localized outbreak, health authorities could deploy these antibodies to protect high-risk individuals in the affected area, creating a biological firewall that prevents the virus from claiming the most vulnerable lives.
Understanding the Impact: A New Era of Viral Management
The discovery of measles-neutralizing antibodies signals a broader trend in medicine: the shift toward precision immunology. We are moving away from “one-size-fits-all” public health measures and toward a system where we have both a broad shield (vaccines) and a precision sword (monoclonal antibodies).
For the general public, the message remains the same: vaccinate. The MMR vaccine is one of the most successful public health interventions in history. However, for the doctor standing in an ICU with a patient who cannot be vaccinated and is struggling to breathe due to measles-induced pneumonia, this research represents a beacon of hope.
The psychological impact of this discovery is also significant. For too long, a measles infection in a vulnerable patient has been a situation of “watch and wait.” By introducing a targeted therapy, we change the narrative from passive observation to active intervention.
Key Takeaways for Patients and Caregivers
- Vaccines are still priority one: No treatment replaces the prevention provided by the MMR vaccine.
- Targeted relief: New research focuses on monoclonal antibodies that block the virus from entering cells.
- Who it helps: The treatment is primarily intended for those who cannot be vaccinated or are already severely ill.
- Passive vs. Active: Vaccines create long-term immunity (active); antibody treatments provide immediate, short-term protection (passive).
- Status: The research is currently in the discovery and pre-clinical stages, moving toward human trials.
Frequently Asked Questions
Can this treatment cure measles if I already have it?
The goal of neutralizing antibodies is to stop the virus from infecting more cells. While it may not “cure” the damage already done to the body, it can stop the virus from spreading further, reduce the severity of the illness, and prevent deadly complications.

Does this mean I don’t need the MMR vaccine?
Absolutely not. The vaccine provides lifelong protection for the vast majority of people. Antibody treatments are temporary and expensive; they are designed as a medical intervention, not a substitute for public health immunization.
When will this treatment be available in hospitals?
It is still in the research and development phase. Before it reaches hospitals, it must pass through several phases of clinical trials to ensure safety and efficacy. This process typically takes several years.
Is this the same as an antiviral drug?
Not exactly. Antiviral drugs usually interfere with the virus’s ability to replicate *inside* the cell. Monoclonal antibodies work *outside* the cell, preventing the virus from ever getting inside in the first place.
Will this help stop the current global outbreaks?
In the long term, yes, by protecting the most vulnerable. However, the only way to stop an outbreak in its tracks is to increase vaccination rates to achieve herd immunity.
The path forward for measles management is now two-pronged. We will continue to fight for every percentage point of vaccination coverage to protect the collective, while simultaneously developing the precision tools necessary to protect the individual. This is the essence of modern medicine: combining the power of public health with the precision of molecular biology.
The next confirmed milestone for this research will be the publication of the first phase of human clinical trial protocols, which will outline the safety parameters and the specific patient cohorts selected for the initial study. We will continue to monitor these developments as they move from the lab to the bedside.
Do you have questions about measles prevention or the future of antibody treatments? Share your thoughts in the comments below or share this article with your community to help spread accurate health information.