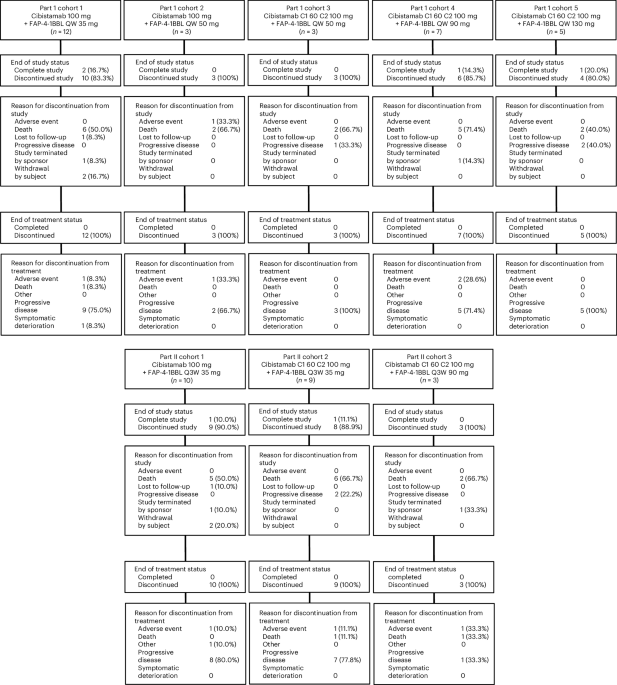
New Immunotherapy Combo Shows Promise in Hard-to-Treat Colorectal Cancer
A phase 1b clinical trial evaluating a novel immunotherapy combination for microsatellite-stable (MSS) colorectal cancer has reported encouraging early results, marking a potential step forward in treating one of the most challenging subtypes of the disease. The study, presented at the 2026 American Association for Cancer Research (AACR) Annual Meeting, investigated the safety and biological activity of combining cibisatamab—a T-cell engager targeting carcinoembryonic antigen (CEA)—with FAP-4-1BBL, a fusion protein designed to stimulate immune activation via the 4-1BB pathway in fibroblasts expressing fibroblast activation protein (FAP).
Microsatellite-stable colorectal cancer accounts for approximately 85% of all colorectal cancer cases and has historically shown limited response to immune checkpoint inhibitors, which have transformed outcomes in microsatellite instability-high (MSI-H) tumors. This therapeutic gap has driven intense interest in alternative immunomodulatory strategies, including bispecific T-cell engagers and agonist antibodies that aim to reprogram the immunosuppressive tumor microenvironment. The trial’s focus on simultaneously targeting CEA-expressing tumor cells and FAP-positive stromal cells reflects a growing interest in dual-action approaches that address both malignant and supportive cells within the tumor niche.
According to trial data shared at AACR 2026, the combination regimen demonstrated a manageable safety profile, with no dose-limiting toxicities observed during the escalation phase. Commonly reported adverse events included mild to moderate cytokine release syndrome, fatigue and transient elevations in liver enzymes—typically resolving with supportive care or temporary treatment interruption. Notably, no Grade 4 or 5 treatment-related adverse events were reported among the 24 patients enrolled in the dose-expansion cohort.
Beyond safety, biomarker analyses revealed signs of immune engagement consistent with the treatment’s mechanistic rationale. Increases in circulating interferon-gamma, granzyme B, and activated CD8+ T cells were detected in a majority of patients following treatment initiation. Immunohistochemical analysis of paired pre- and post-treatment biopsies showed increased T-cell infiltration into tumor stroma and reduced FAP-expressing fibroblast density in several cases, suggesting modulation of the tumor microenvironment.
While objective tumor responses per RECIST v1.1 criteria were limited—consistent with early-phase immunotherapy trials in MSS colorectal cancer—stable disease was observed in 11 patients (approximately 46%) at the first radiographic assessment, with a median duration of stable disease of 4.2 months. Researchers emphasized that these findings support further investigation, particularly in biomarker-selected populations or in combination with other immunomodulatory agents.
Understanding the Science Behind the Combination
Cibisatamab is a bispecific T-cell engager designed to bind both CD3 on T cells and CEA, a glycoprotein frequently overexpressed in colorectal adenocarcinoma. By physically linking T cells to tumor cells, cibisatamab aims to redirect cytotoxic T-lymphocyte activity against malignant cells regardless of their antigen presentation status—a strategy intended to overcome some limitations of traditional checkpoint blockade.
FAP-4-1BBL, meanwhile, targets fibroblast activation protein (FAP), which is upregulated in cancer-associated fibroblasts within the stromal compartment of many solid tumors, including colorectal cancer. The fusion protein delivers the 4-1BBL ligand—a key co-stimulatory signal for T-cell survival, proliferation, and effector function—directly to the tumor microenvironment. By engaging 4-1BB on tumor-infiltrating lymphocytes, FAP-4-1BBL seeks to enhance and sustain T-cell activity while potentially counteracting immunosuppressive signals from stromal cells.
The rationale for combining these agents lies in addressing two complementary barriers to effective anti-tumor immunity: the need to effectively engage T cells with tumor cells (via cibisatamab) and the need to counteract an immunosuppressive stroma that can inhibit T-cell function and persistence (via FAP-4-1BBL). Preclinical models have shown that dual targeting can lead to synergistic T-cell activation and tumor regression in settings where either agent alone shows limited efficacy.
Experts not involved in the trial noted that while the approach is biologically sound, translating such combinations into durable clinical benefit remains challenging. “The tumor microenvironment in MSS colorectal cancer is notably resistant to immune infiltration,” said Dr. Lena Meyer, an oncologist specializing in gastrointestinal malignancies at Heidelberg University Hospital, in an interview following the AACR presentation. “Strategies that simultaneously target tumor cells and modulate stromal support represent a logical next step, but we need longer follow-up and larger cohorts to determine whether this translates into meaningful clinical outcomes.”
Context Within Broader Immunotherapy Efforts
This trial adds to a growing body of research exploring immunomodulatory strategies for MSS colorectal cancer, a disease that has lagged behind MSI-H counterparts in benefiting from the immunotherapy revolution. While pembrolizumab and nivolumab have become standard-of-care options for MSI-H metastatic colorectal cancer—based on landmark trials showing improved progression-free and overall survival—similar benefits have not been consistently observed in MSS disease.
Other investigational approaches being studied include cancer vaccines, adoptive T-cell therapies, and combinations targeting immunosuppressive pathways such as TGF-β, IL-10, or prostaglandin E2. Several trials are also evaluating whether priming the tumor microenvironment with radiation, chemotherapy, or oncolytic viruses can improve susceptibility to subsequent immunotherapy.
The sponsors of the cibisatamab and FAP-4-1BBL trial have indicated plans to advance the combination into a phase 2 study, pending further analysis of biomarker-correlated outcomes and safety data. No official start date or enrollment targets for a follow-up study have been publicly disclosed as of May 2026.
What This Means for Patients and Clinicians
For patients with microsatellite-stable colorectal cancer—particularly those who have exhausted standard chemotherapy and targeted therapy options—the availability of novel immunomodulatory strategies offers hope for future treatment avenues. While the current data do not support routine clinical use outside of research settings, the trial contributes to a deeper understanding of how combination immunotherapy might be optimized for immunologically “cold” tumors.
Clinicians managing gastrointestinal malignancies are advised to stay informed about ongoing clinical trials through registries such as ClinicalTrials.gov and the European Clinical Trials Register. Patients interested in participating in investigational therapies should discuss eligibility with their oncology care team, as trial participation often depends on prior treatment history, tumor biomarker status, and organ function.
Ongoing monitoring of immune-related adverse events remains essential, even with regimens that appear well-tolerated in early phases. Guidelines from organizations such as the European Society for Medical Oncology (ESMO) and the National Comprehensive Cancer Network (NCCN) recommend heightened vigilance for signs of cytokine release syndrome, colitis, hepatitis, and endocrinopathies when administering T-cell engaging therapies.
As research continues, the emphasis remains on identifying biomarkers that may predict response to such combinations—whether based on baseline immune infiltrate, FAP expression levels, CEA heterogeneity, or genetic profiles. Future trials may also explore sequencing strategies, such as administering FAP-4-1BBL prior to or concurrently with cibisatamab, to optimize immune priming.
The next major opportunity to review updated data from this investigation is expected at the 2026 European Society for Medical Oncology (ESMO) World Congress on Gastrointestinal Cancer, scheduled for June 26–29, 2026, in Barcelona, Spain. Abstract submission deadlines for the conference closed in April 2026, with presenting authors notified of acceptance in May.
We encourage readers to share their thoughts and questions in the comments below. If you found this article informative, please consider sharing it with others who may benefit from updates on advancing cancer research.